A panniculectomy, also known as an apronectomy, is a surgical procedure designed to remove excess skin and tissue of the lower abdomen that hangs below the waistline, called the pannus. The procedure may help address physical concerns such as skin irritation, hygiene issues, or limitations in movement, depending on the tissue involved.
In contrast to a tummy tuck, a panniculectomy focuses on removing overhanging skin but does not tighten abdominal muscles or address excess skin in the upper abdomen.
At the CREO Clinic, panniculectomy is performed by Dr Omar Tillo, our Medical Director and body-contouring specialist, following a consultation-led assessment to determine whether this approach is clinically appropriate.
Why this procedure matters
Significant laxity of the abdominal skin following rapid weight loss or pregnancy often does not respond to exercise or other lifestyle changes. These changes are typically related to structural alterations in the skin and underlying tissues, which may lead to rashes, infections, or hygiene issues in skin folds.
A panniculectomy can directly address these issues by permanently removing the skin folds.
Completing a post-weight loss transformation
In patients who have undergone substantial weight loss, a panniculectomy may form part of a staged surgical plan, addressing residual excess skin once weight has stabilised and suitability has been confirmed through clinical assessment.
Restoring comfort and mobility
Overhanging abdominal skin can contribute to physical discomfort and restrictions in movement. In selected cases, removing this tissue may help reduce these limitations, although outcomes depend on the degree of tissue excess and patient-specific factors.
Addressing persistent excess abdominal skin
Once skin elasticity has been lost, non-surgical options are typically limited. A panniculectomy may be considered where excess tissue is stable, although long-term outcomes depend on maintaining weight stability and avoiding further factors that affect skin integrity.
What is a panniculectomy?
A panniculectomy removes the overhanging fold of lax skin around the lower abdomen, often caused by pregnancy or significant weight loss. The procedure does not address diastasis recti or improve the abdominal contour – for this, an abdominoplasty (tummy tuck) is more appropriate.
The table below provides a clearer picture of what each surgery does and doesn’t involve:
| Feature | Tummy Tuck | Panniculectomy |
| Removes excess lower abdominal skin | ✓ | ✓ |
| Removes upper abdominal skin | ✓ (Reverse tummy tuck) | ╳ |
| Tightens abdominal muscles | ✓ | ╳ |
| Repositions the umbilicus | ✓ (If necessary) | ╳ |
| Creates horizontal hip-to-hip scar | ✓ | ✓ |
| Addresses abdominal contour | ✓ | ╳ |
| Primarily for purely medical indications | ╳ | ✓ |
| Can be combined with tummy tuck elements | N/A | ✓ |
How the procedure works
Surgical technique
In a typical panniculectomy, an incision is made across the lower abdomen from hip to hip. The exact incision pattern may vary depending on the volume and distribution of excess skin, as well as individual anatomical considerations. In some cases, additional incisions along the flanks may be required to achieve an appropriate contour. The excess skin is removed, and the remaining tissue is sutured using established surgical techniques, with dressings applied to support healing.
Anaesthesia and procedure duration
A panniculectomy is performed under general anaesthesia and typically lasts for 2-3 hours. The duration of the surgery can vary depending on the extent of tissue removal and surgical complexity, and the need for an overnight stay is determined based on intraoperative findings and early recovery.
Operating environment and clinical safety
All surgeries at the CREO Clinic are performed in CQC-registered surgical facilities. Experienced clinicians and anaesthetists are present throughout the procedure and during post-surgical monitoring.
Is this procedure right for you?
Whether a panniculectomy is suitable for you will depend on your clinical consultation with Dr Tillo, during which he will assess your suitability and make his clinical recommendation.
Who’s it for
Panniculectomy is a targeted surgery and is only appropriate for a defined group of patients following clinical evaluation.
It may be appropriate for patients who:
- Have significant excess lower abdominal skin, causing physical issues, such as skin irritation, hygiene issues, or limited movement
- Have a stable BMI (ideally below 30) and are close to their ideal weight. Use our BMI Calculator to check
- Have realistic expectations about outcomes, with an understanding that scarring is an inevitable consequence of the surgery
Who it may not be right for
The procedure is unlikely to be appropriate for patients who:
- Are active smokers, or feel unable to quit for the four weeks before surgery
- Have ongoing weight fluctuation or a BMI above 30, where outcomes may be less predictable
- Require abdominal muscle repair or full contouring, where an abdominoplasty may be more suitable
- Have medical conditions that significantly increase surgical or anaesthetic risk, as determined during consultation
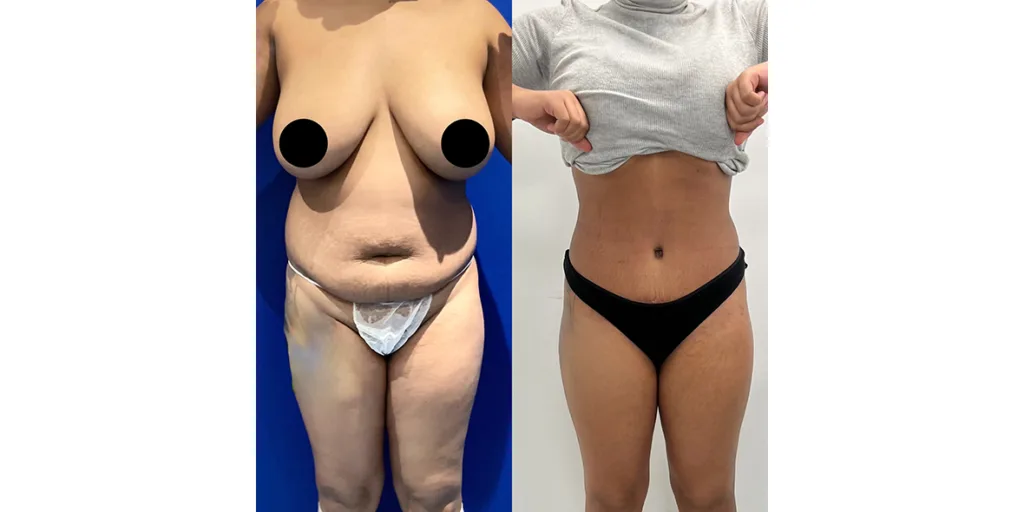
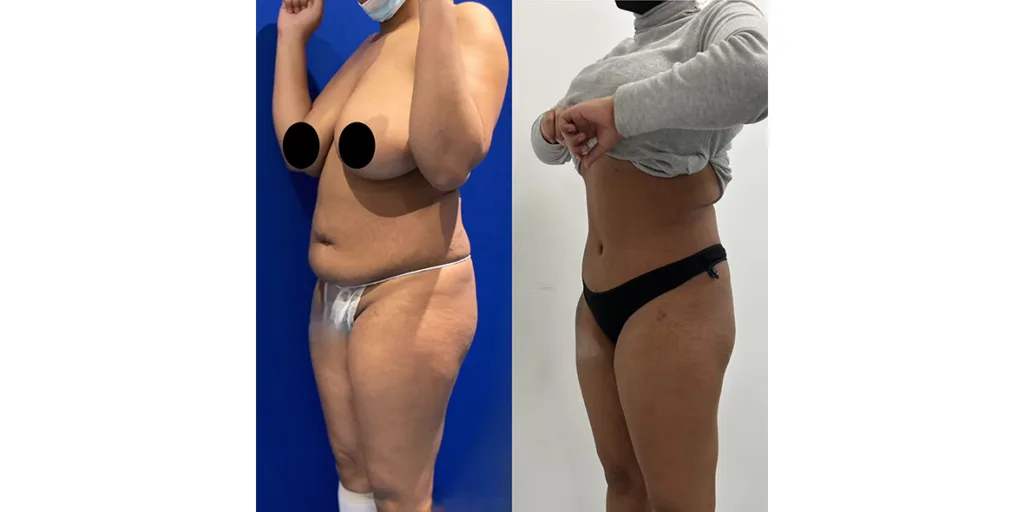
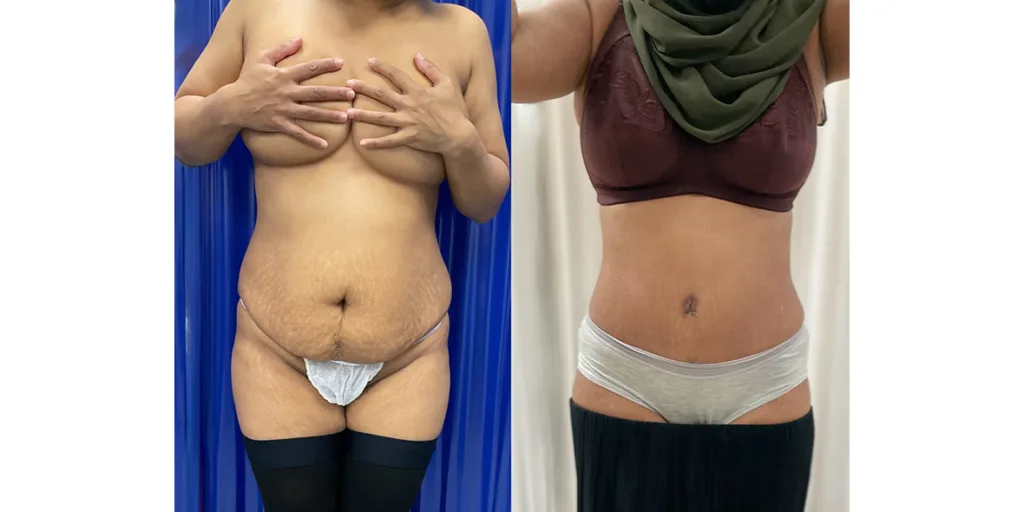
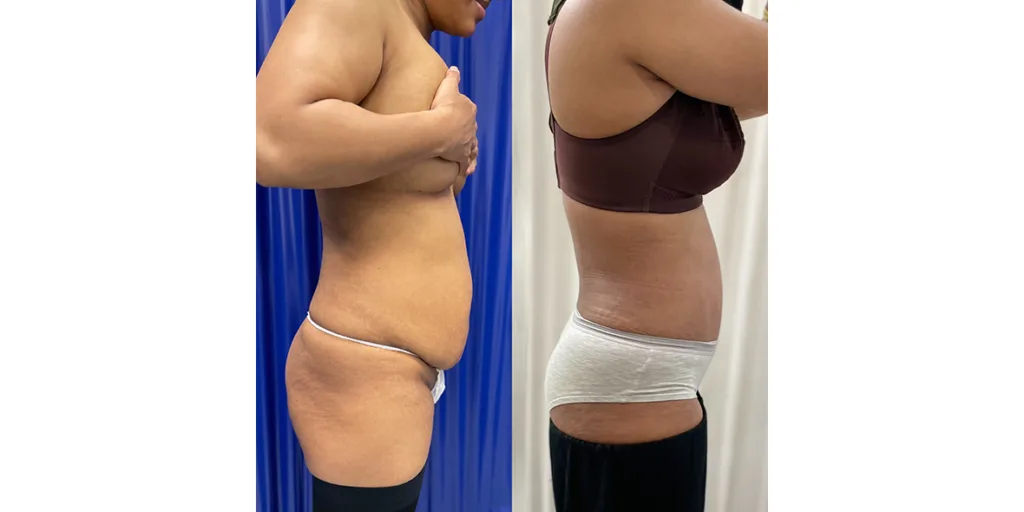
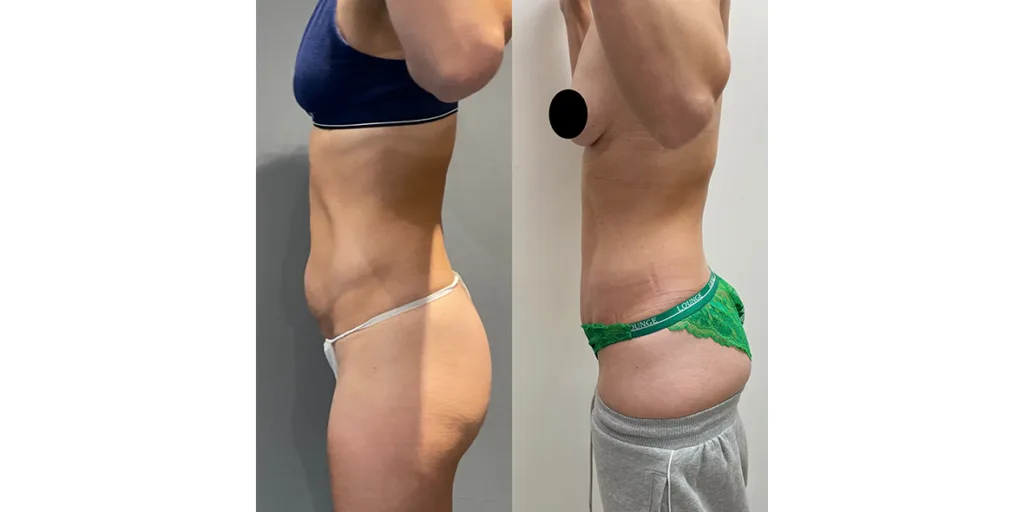
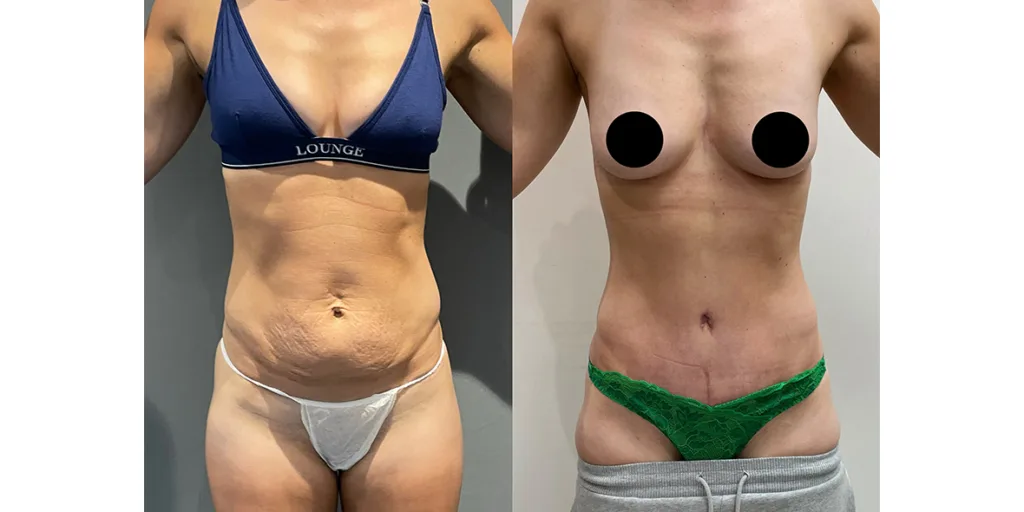
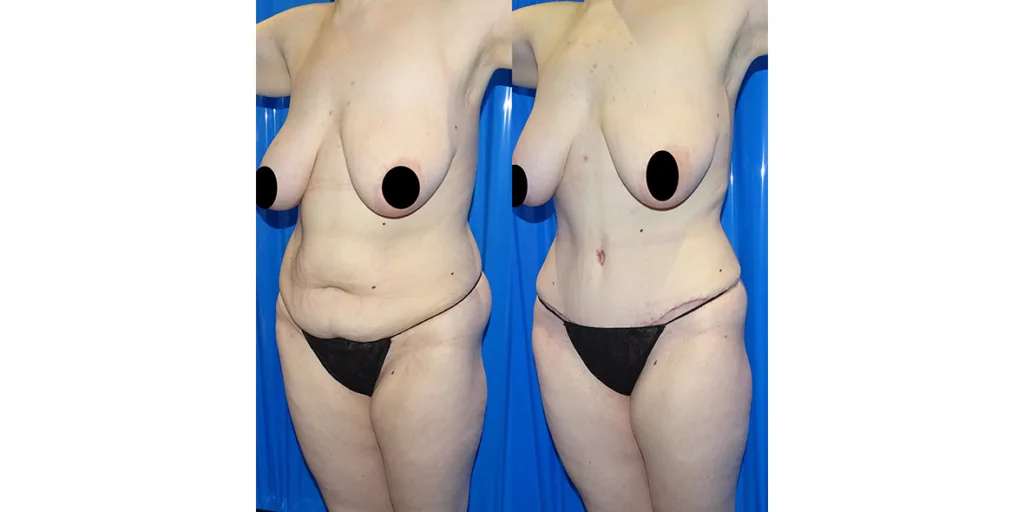
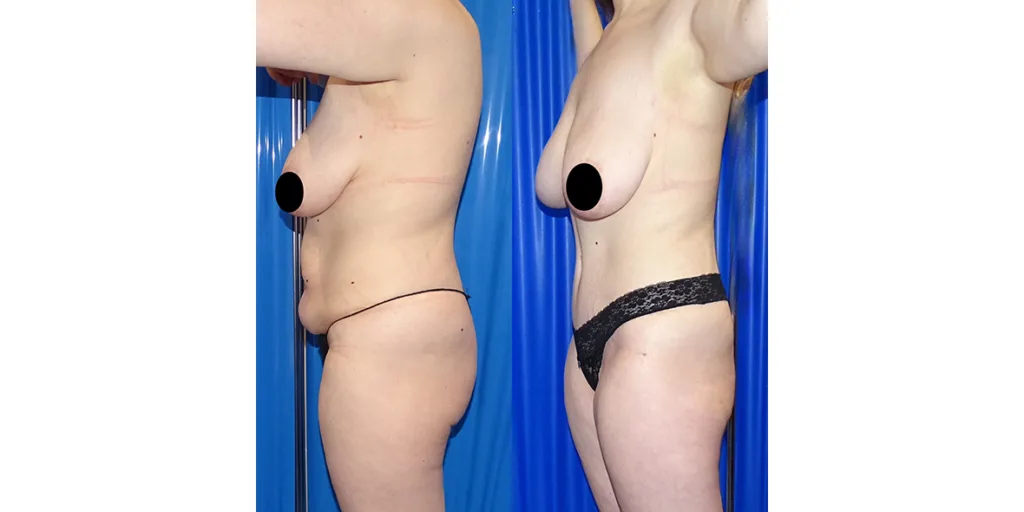
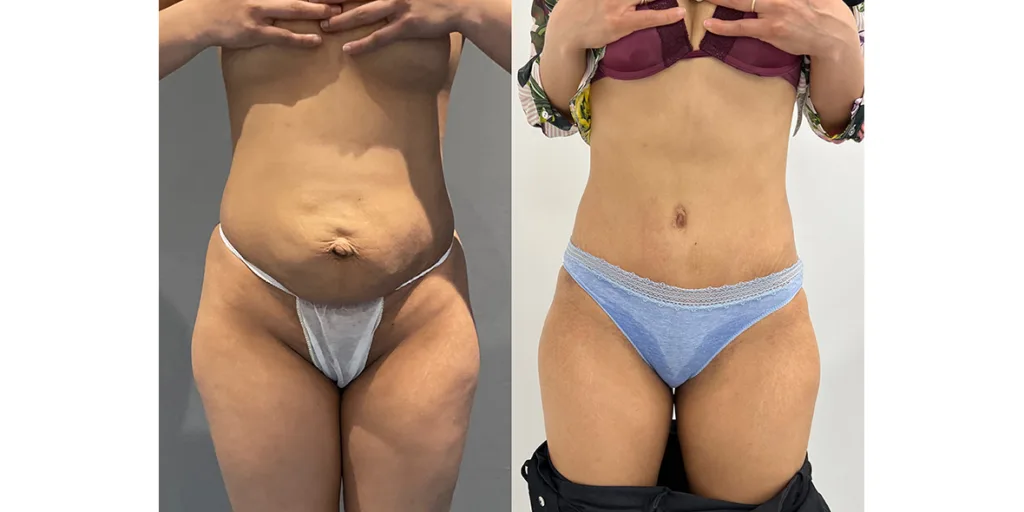
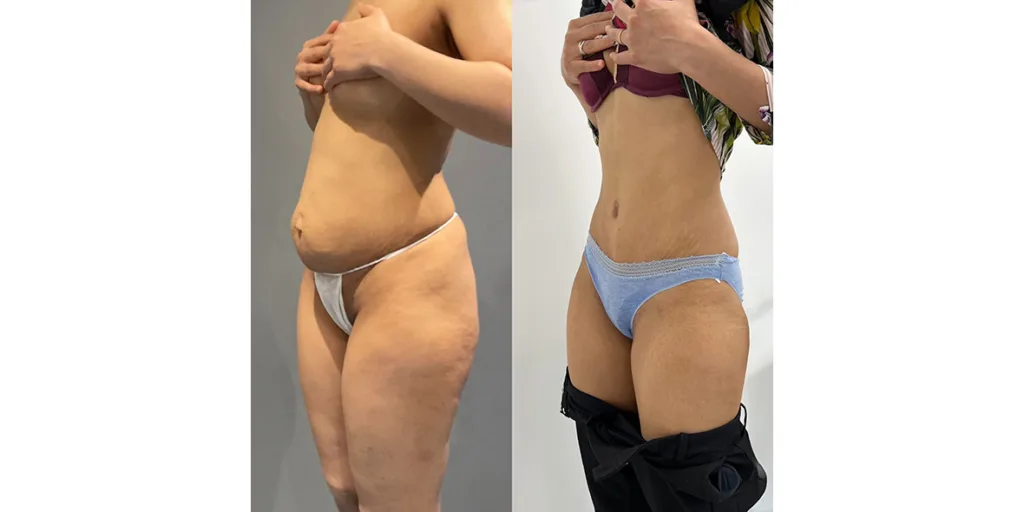
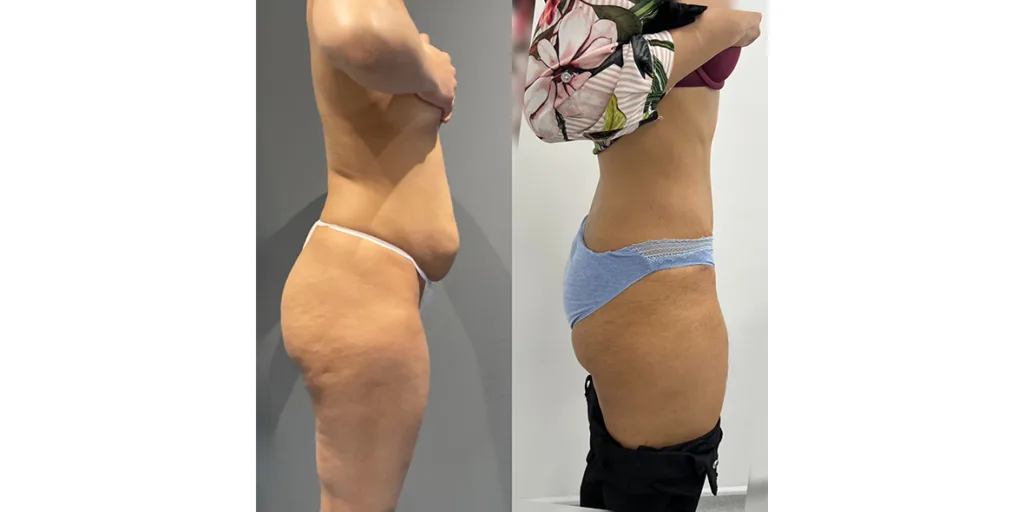
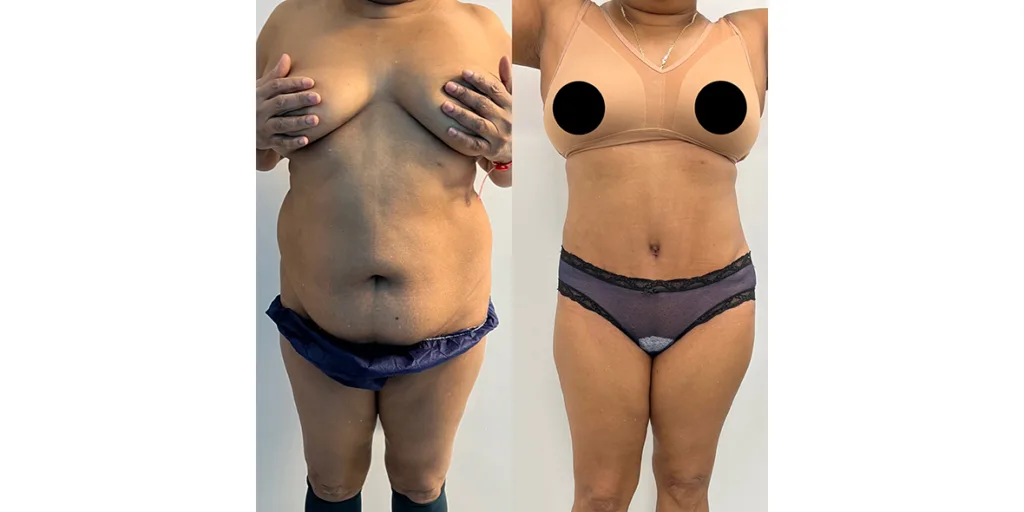
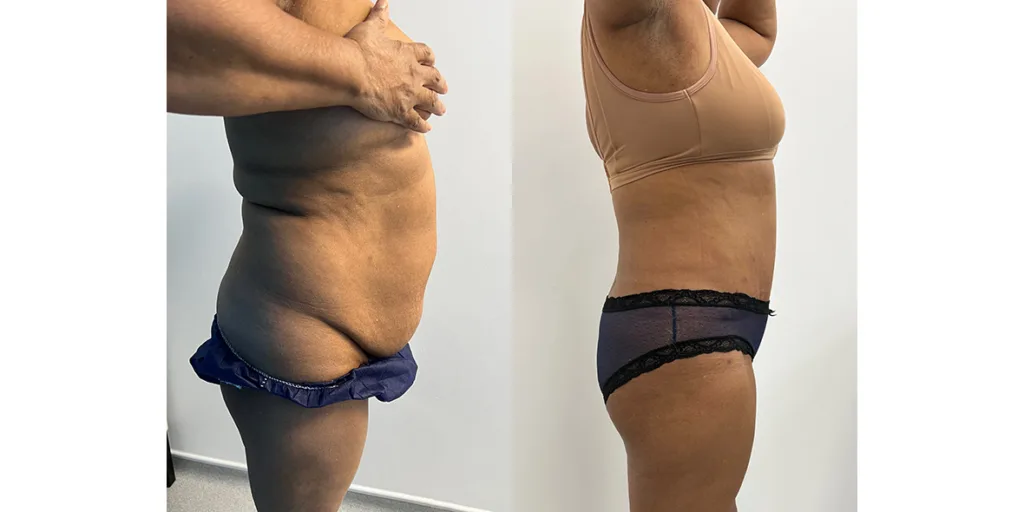
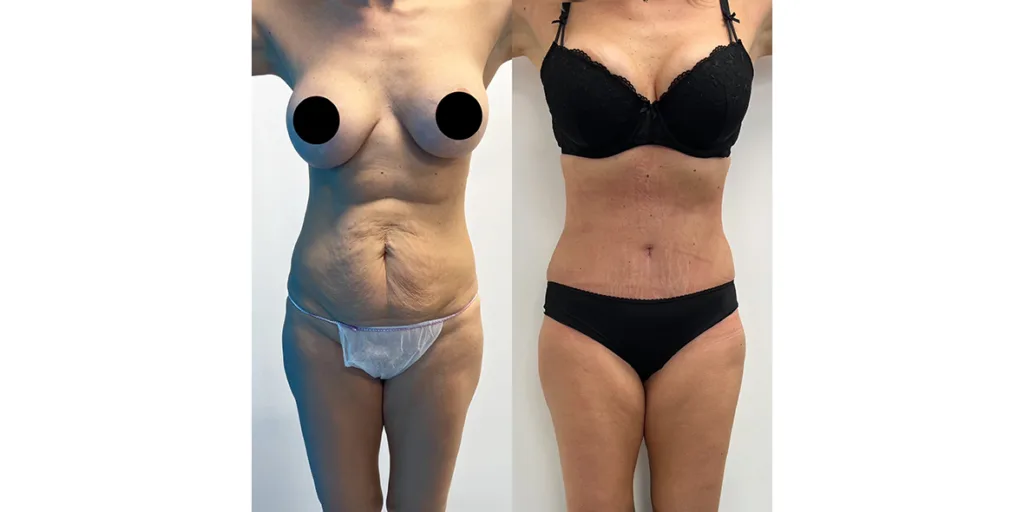
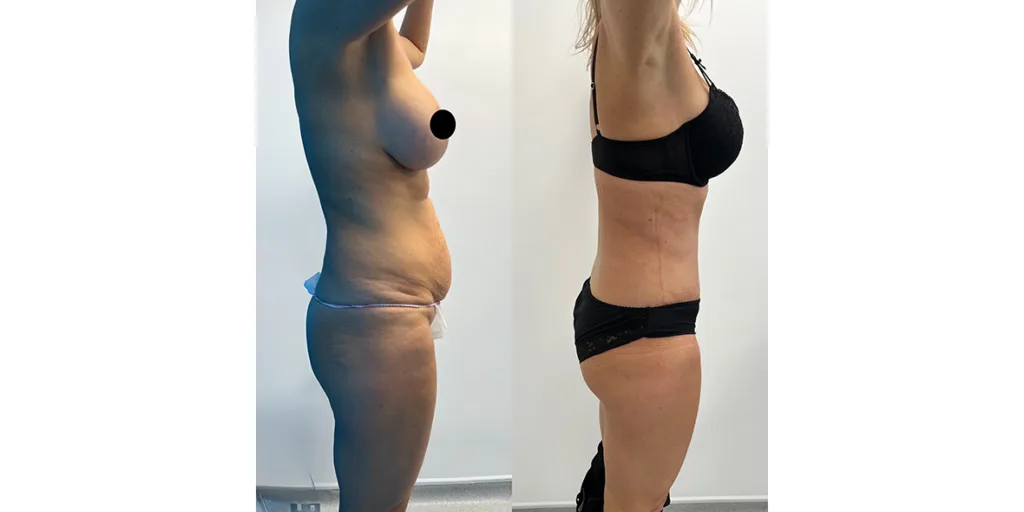
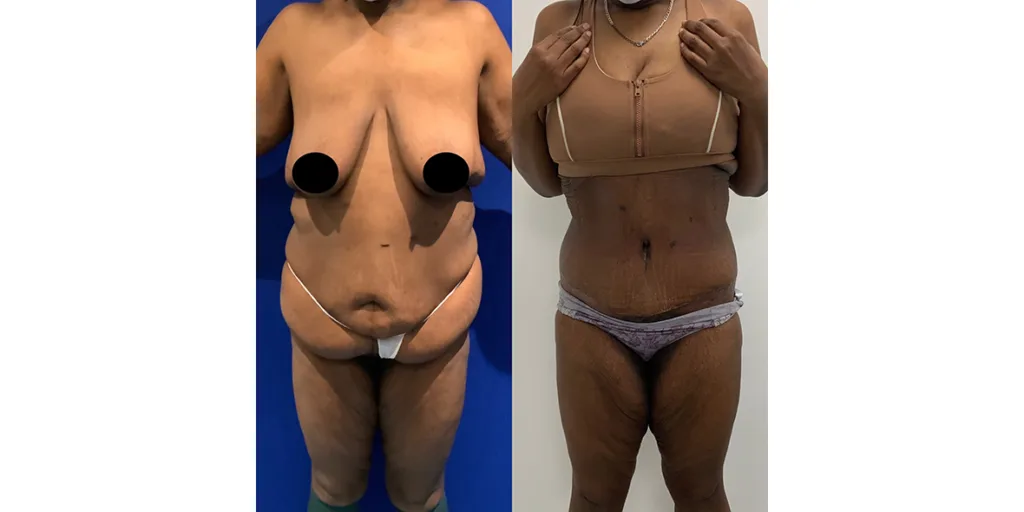
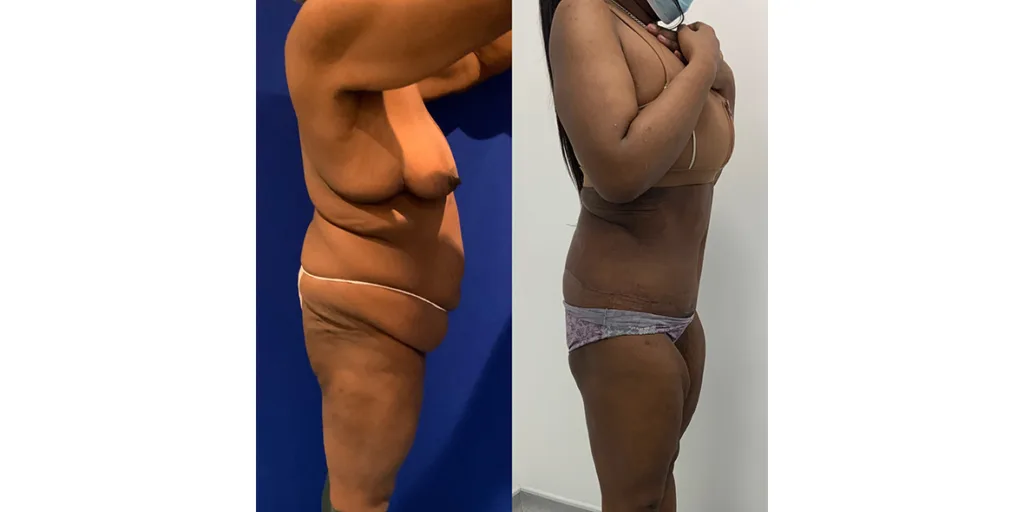
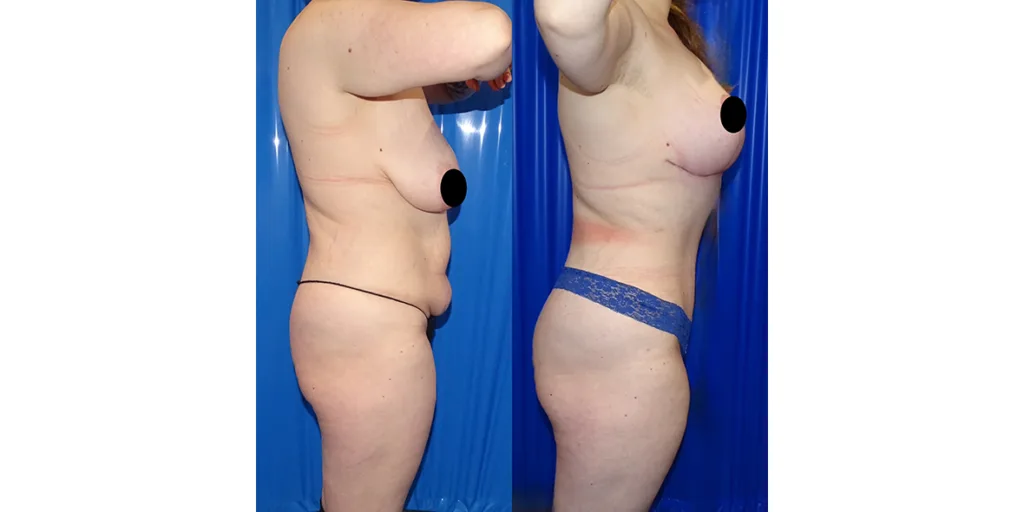
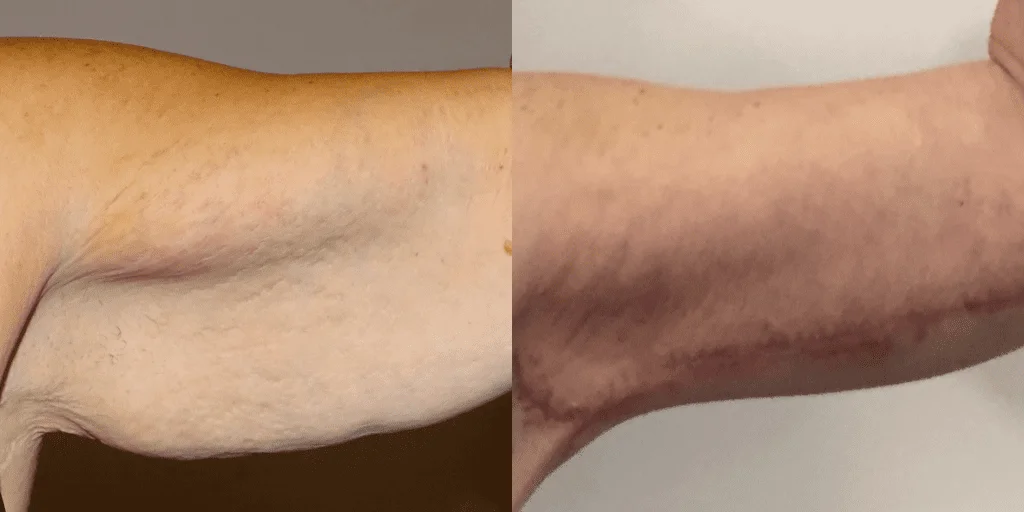
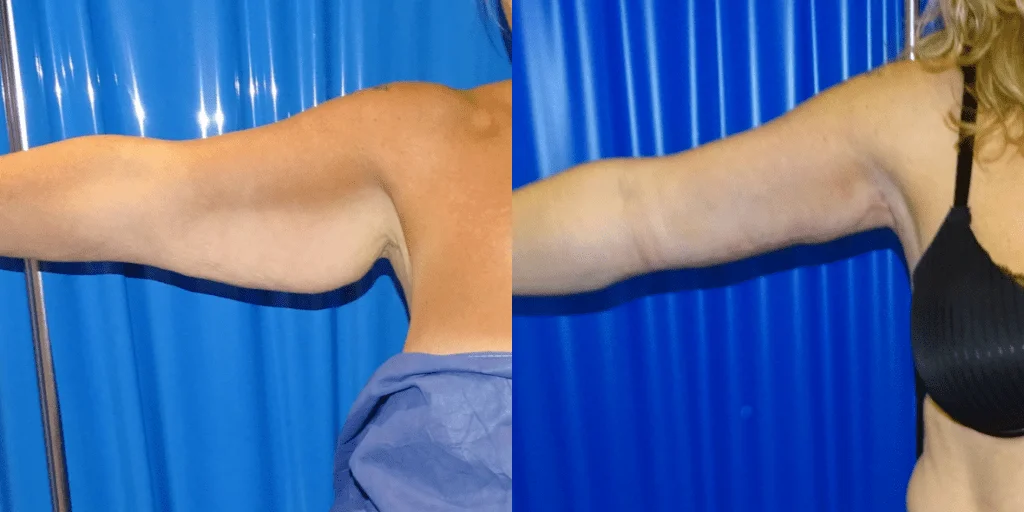
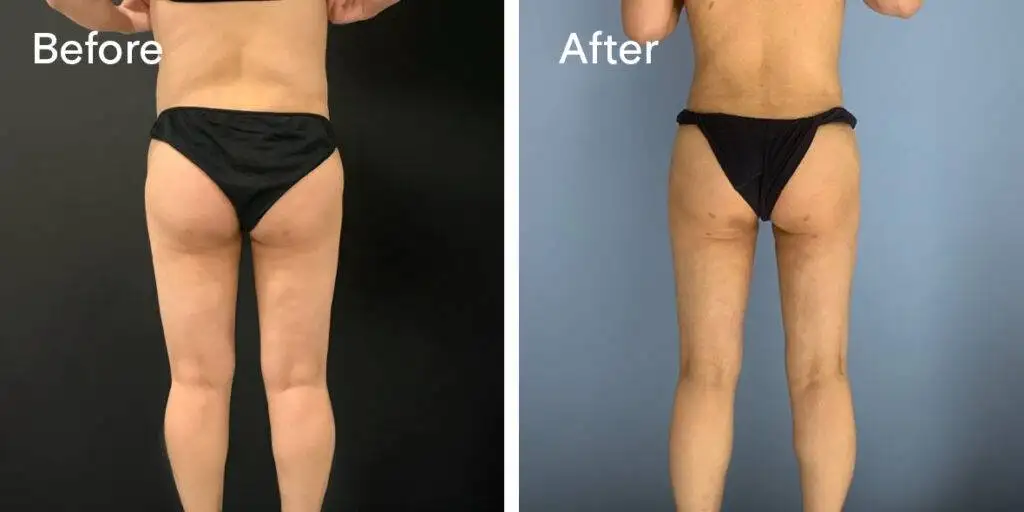
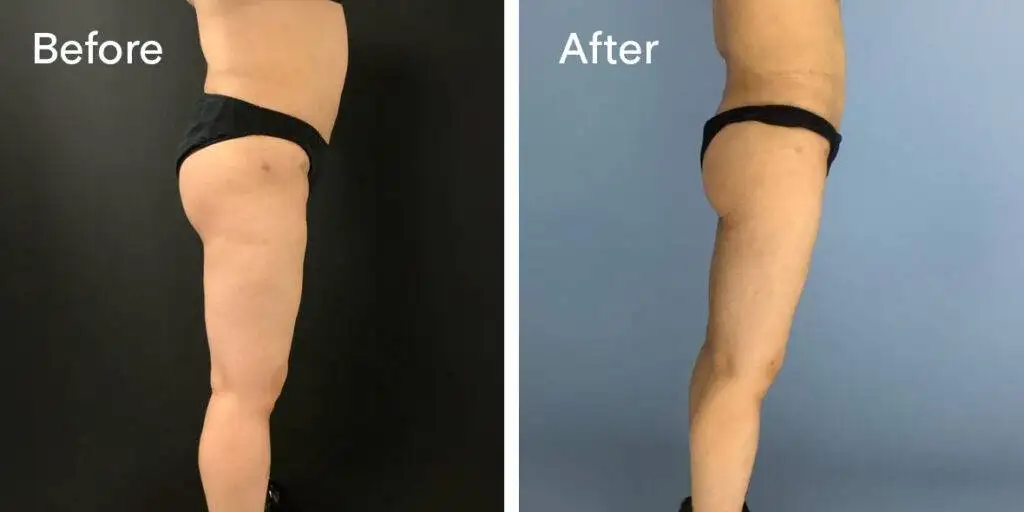
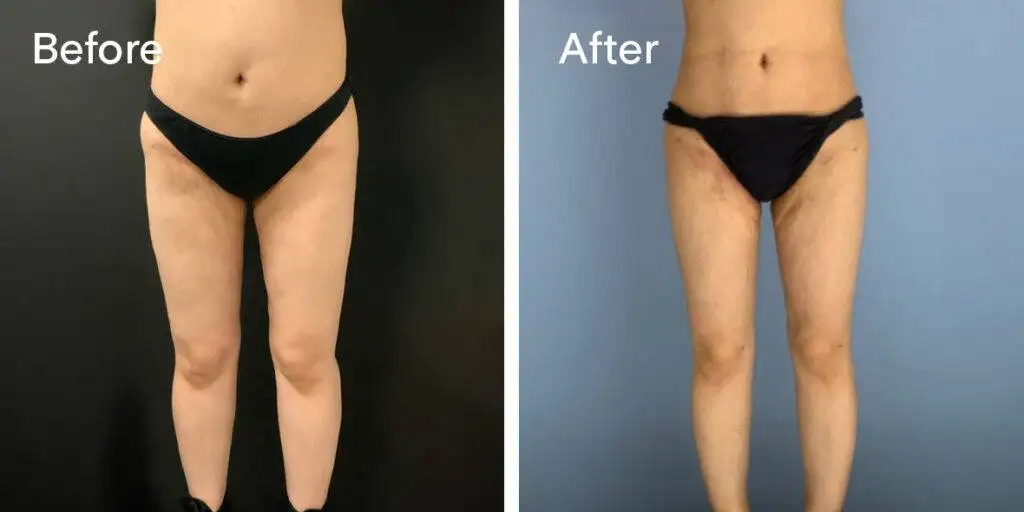
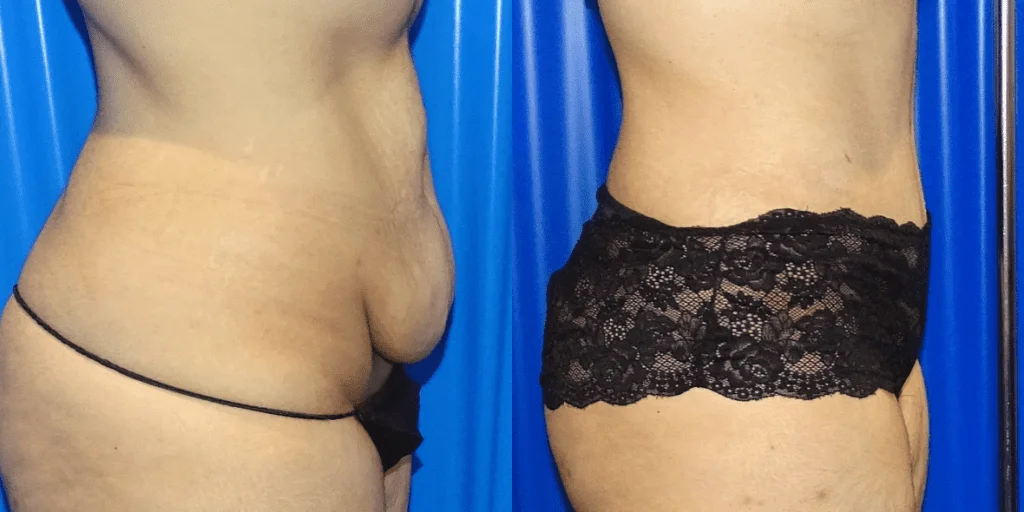
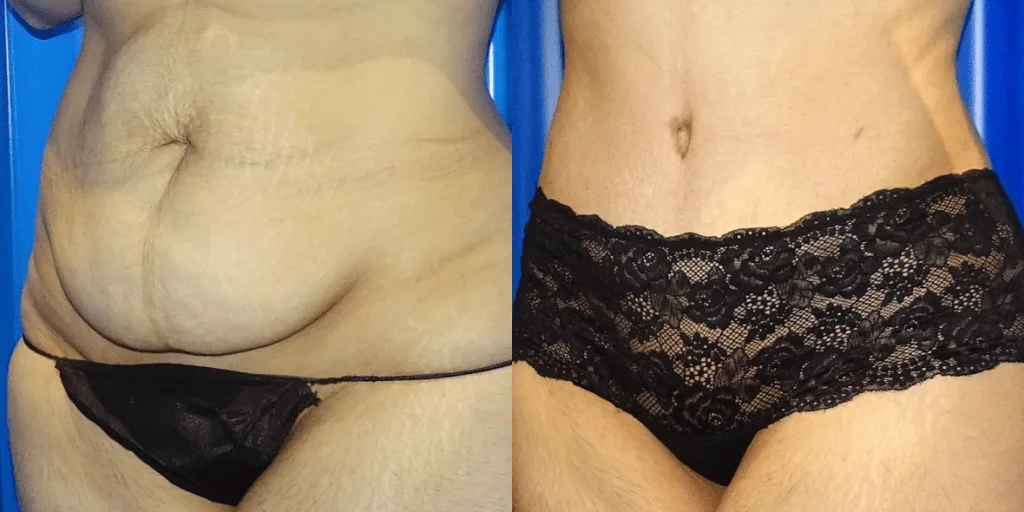
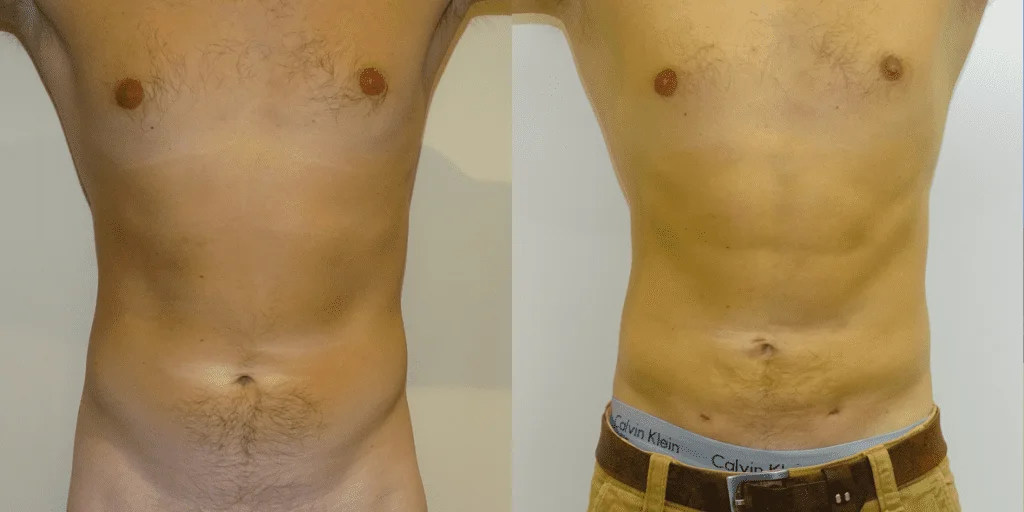
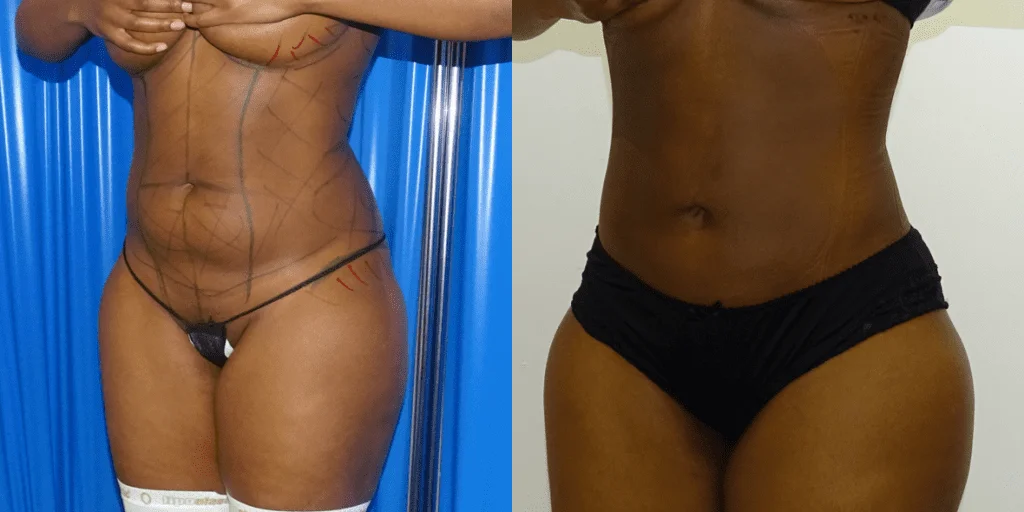
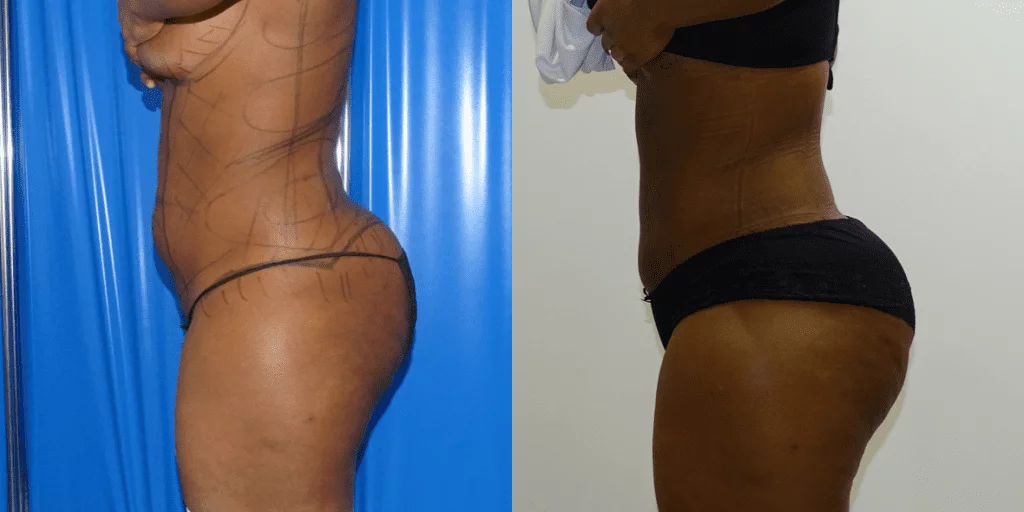
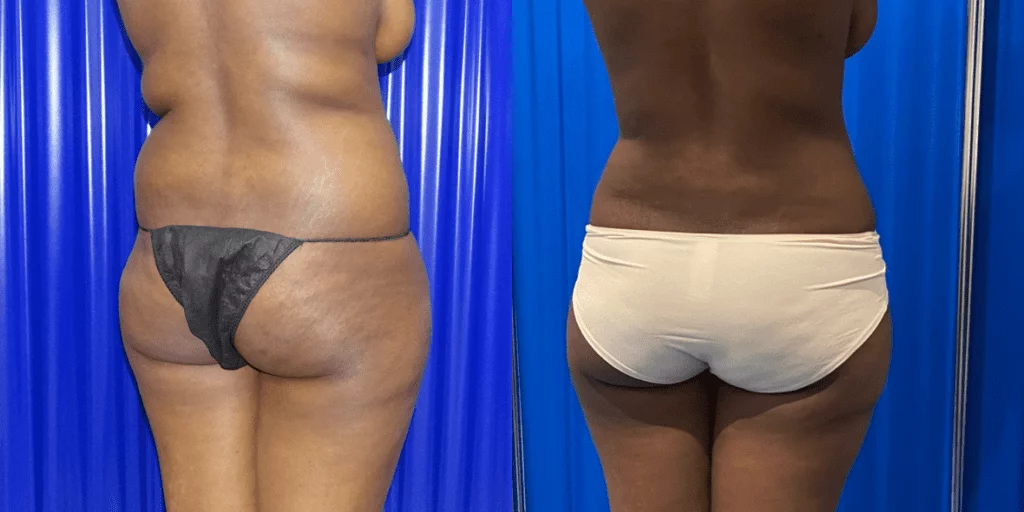
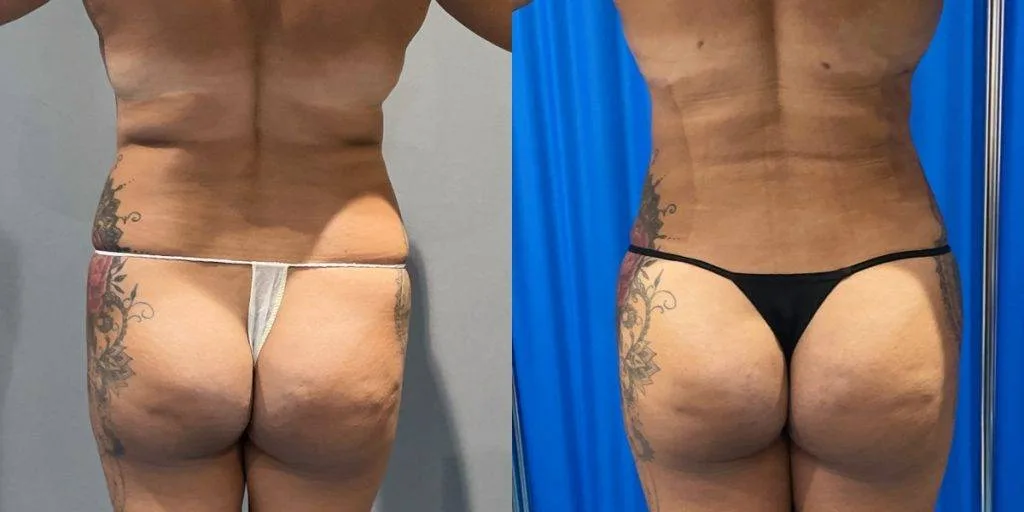
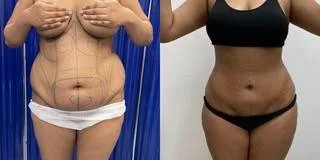
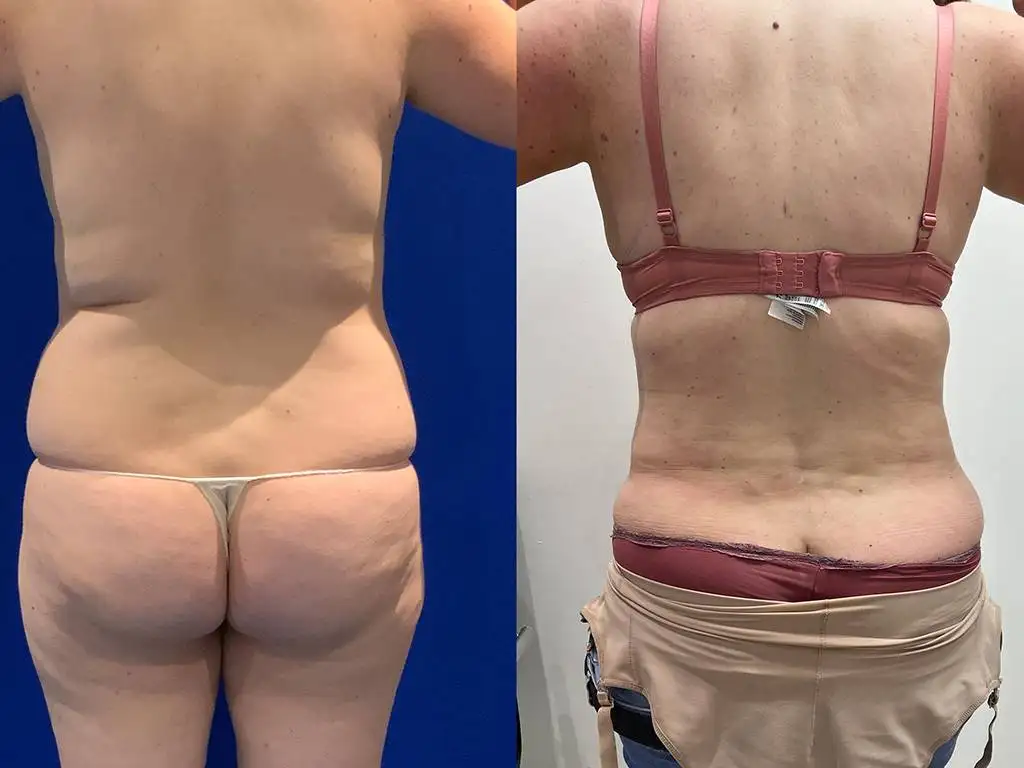
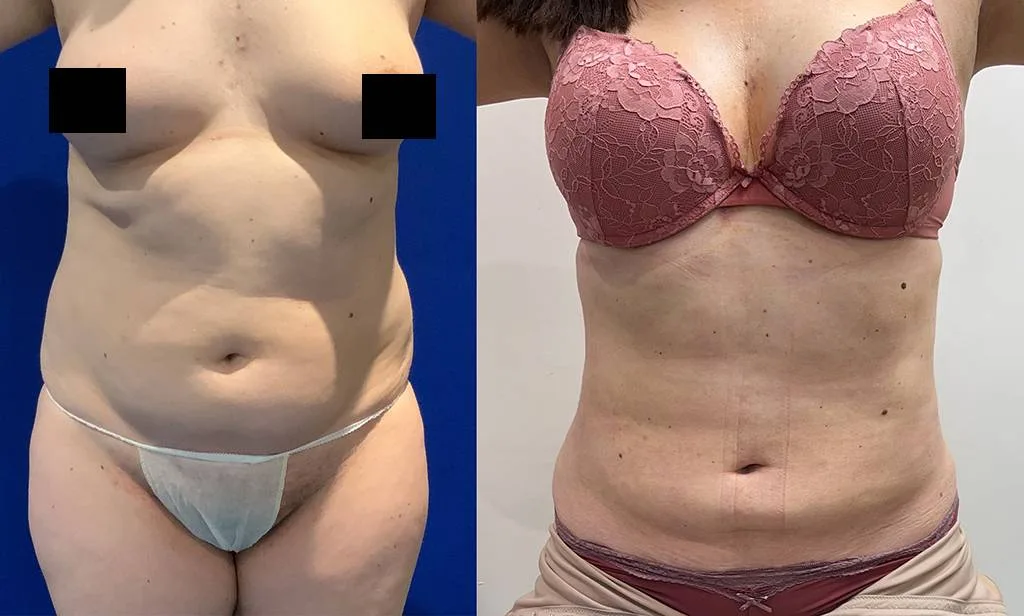
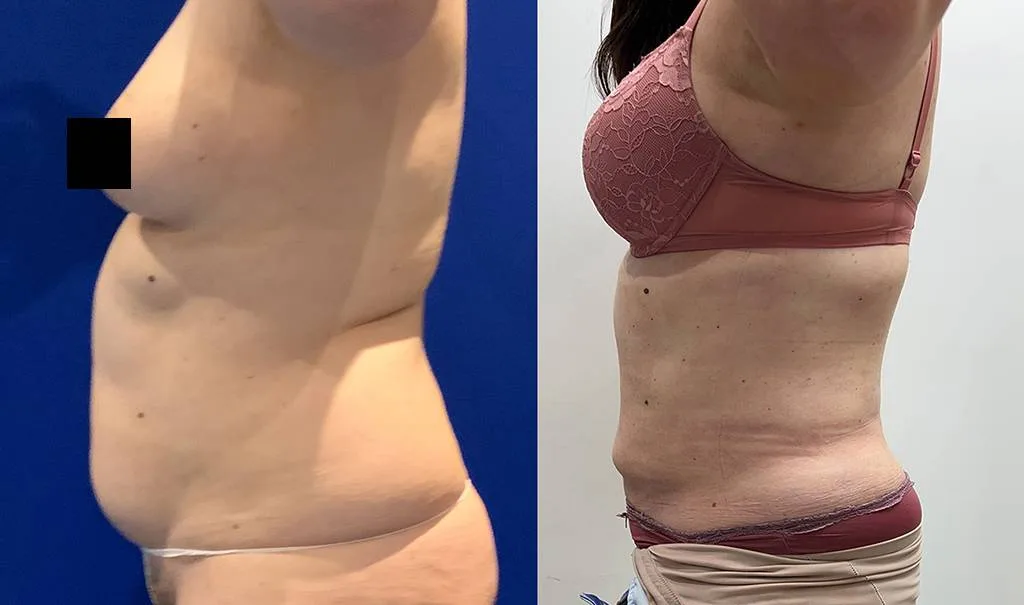
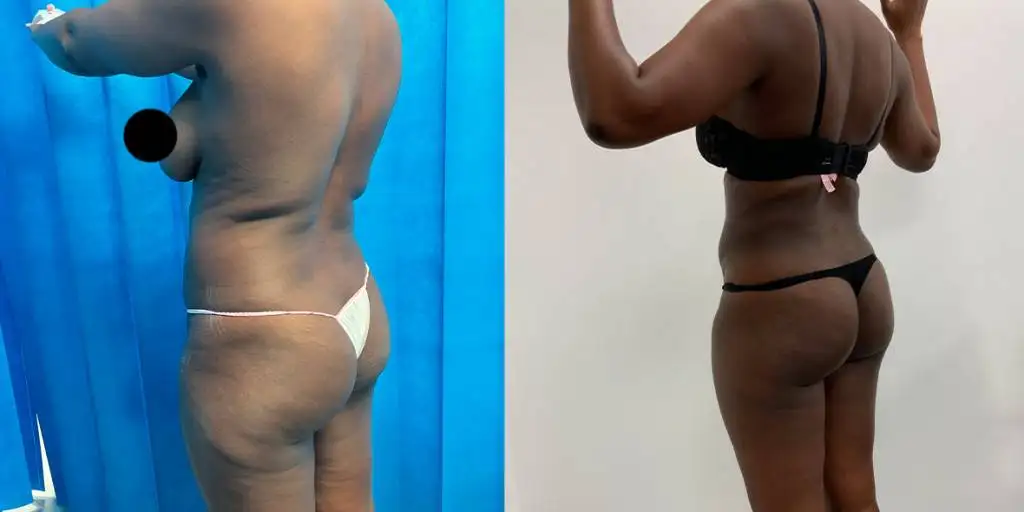
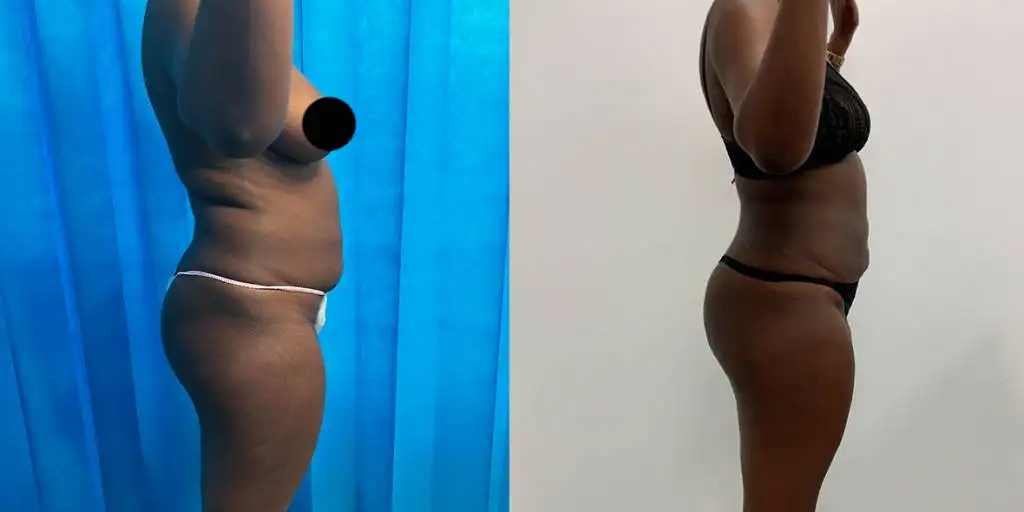
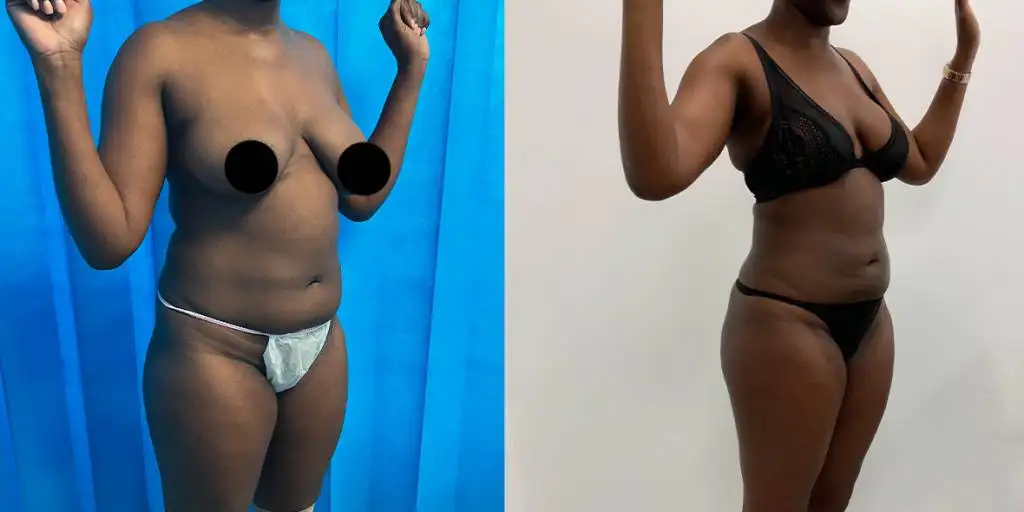
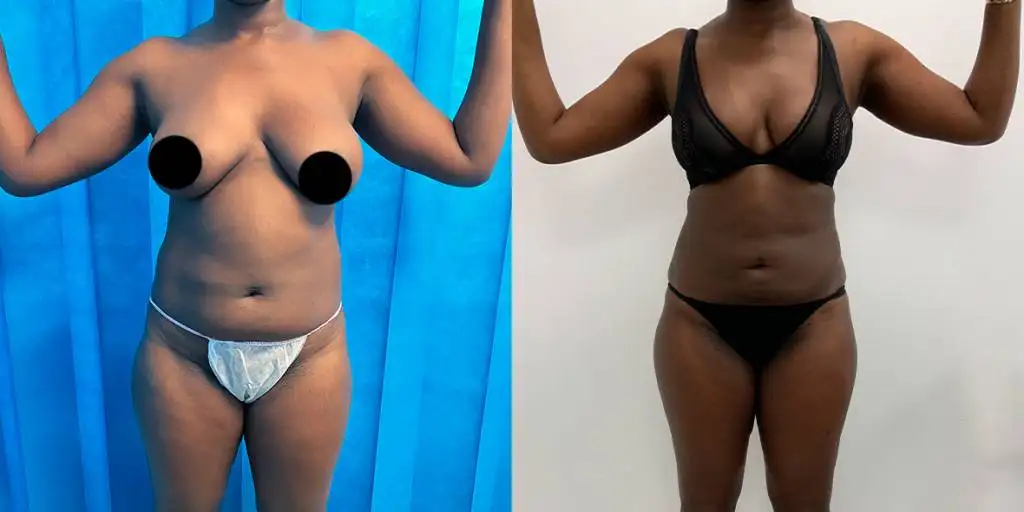
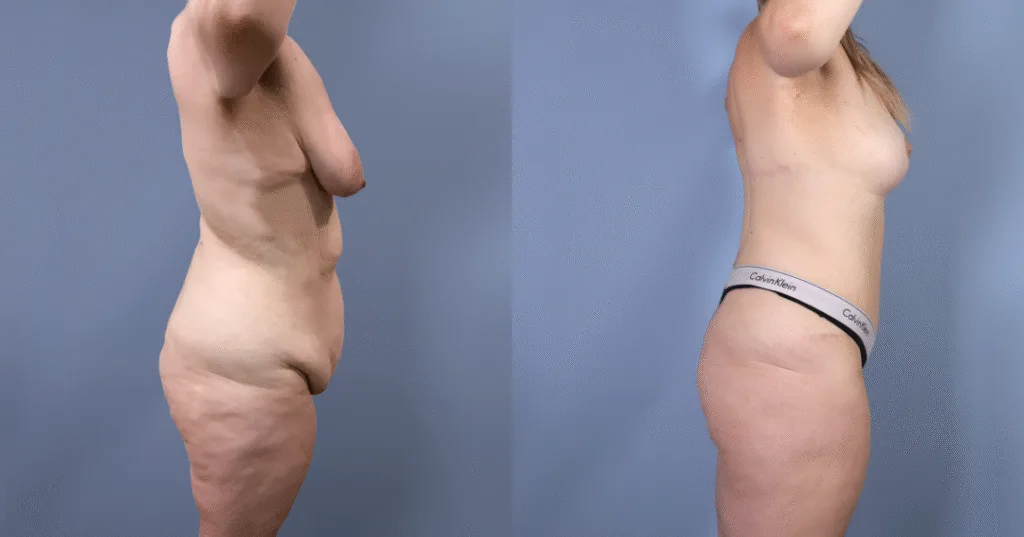
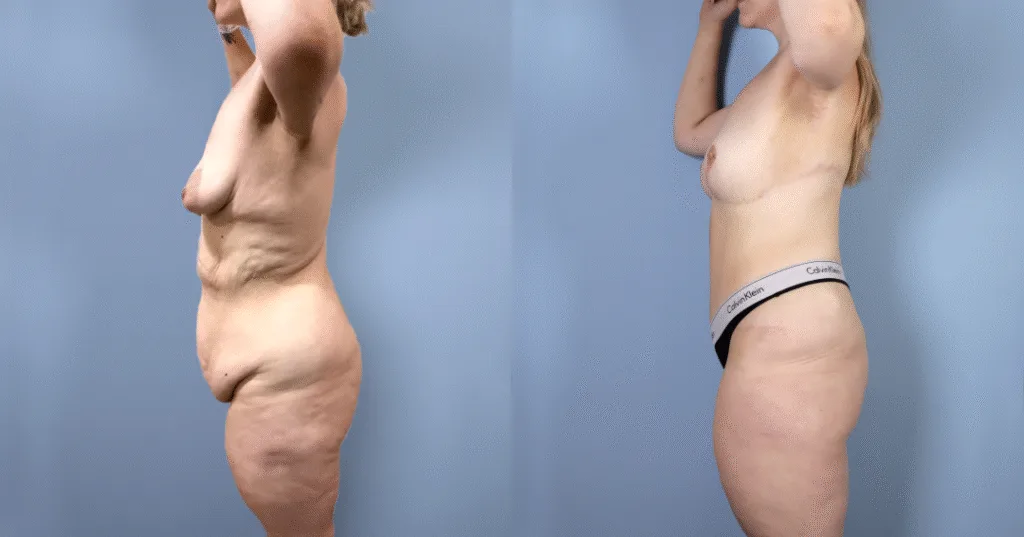
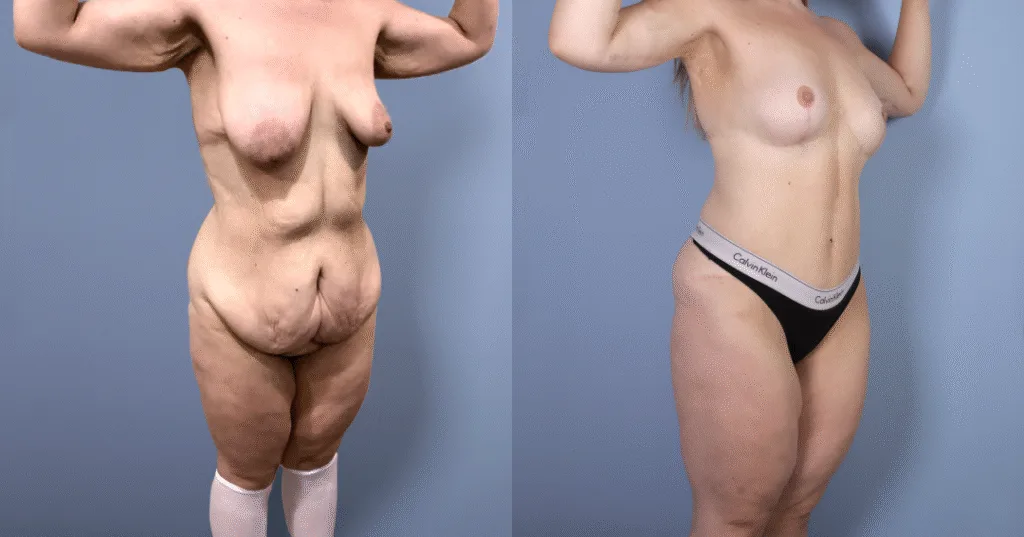
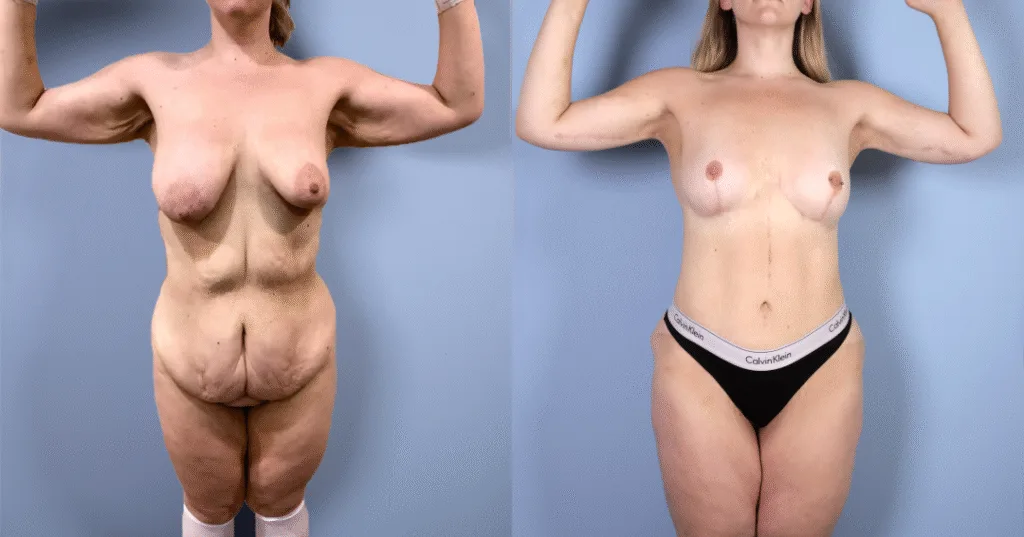
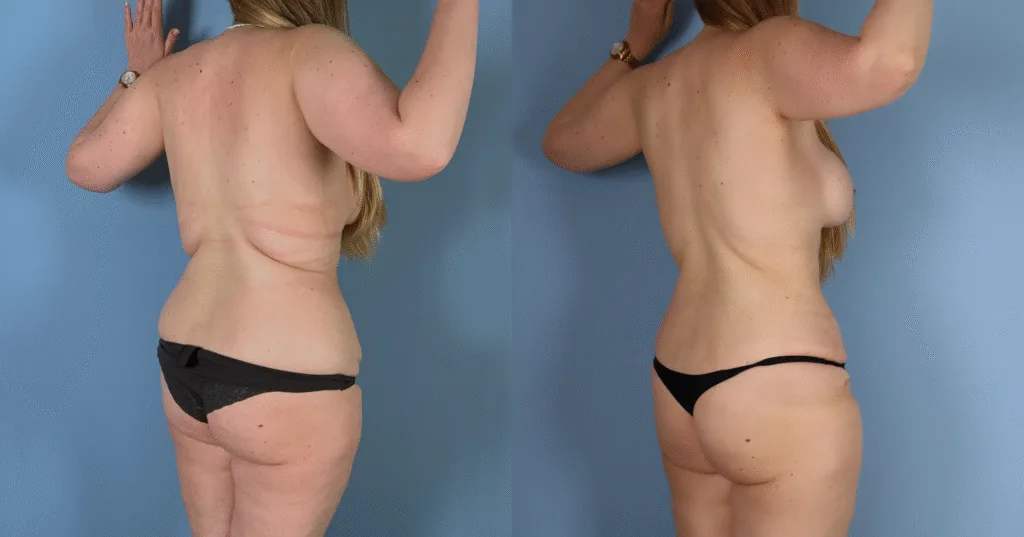
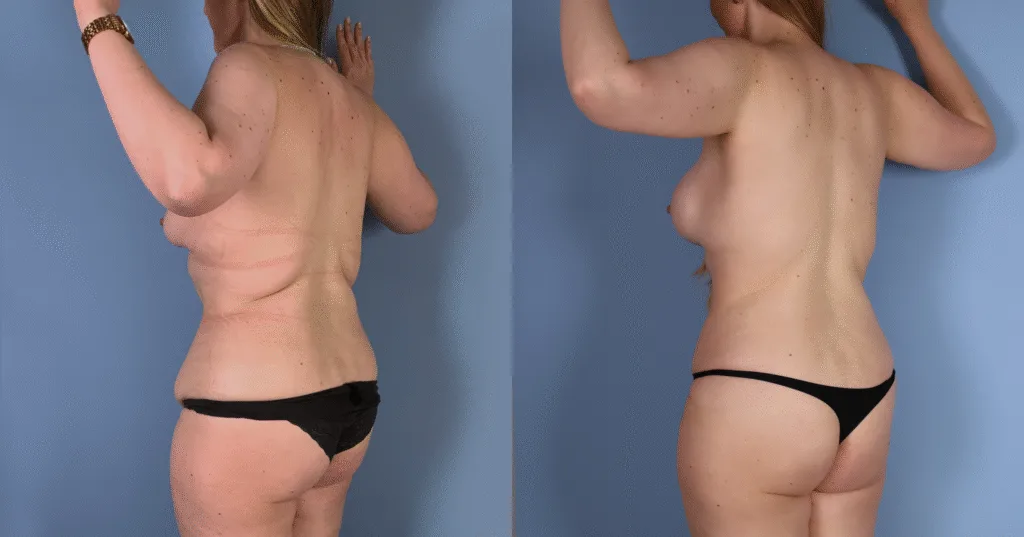
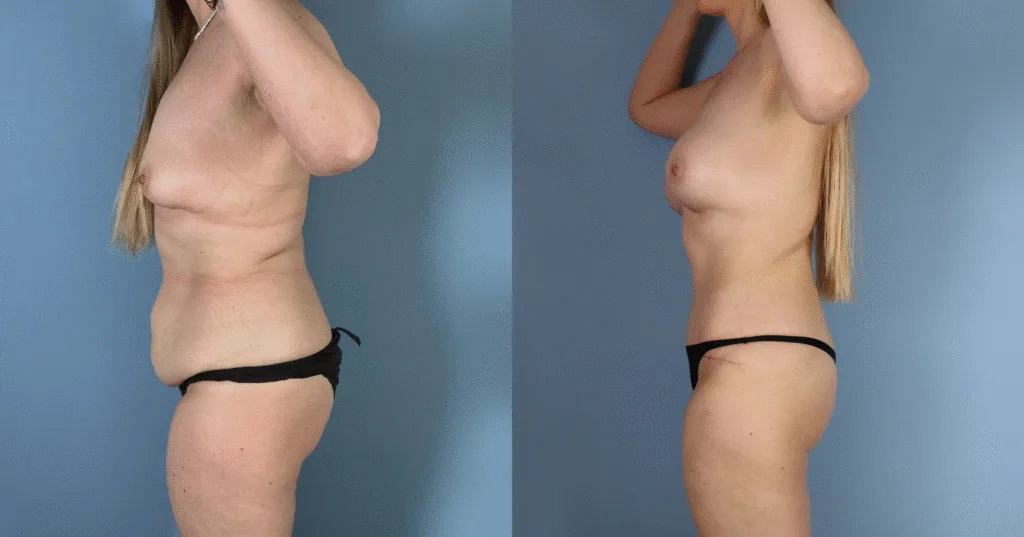
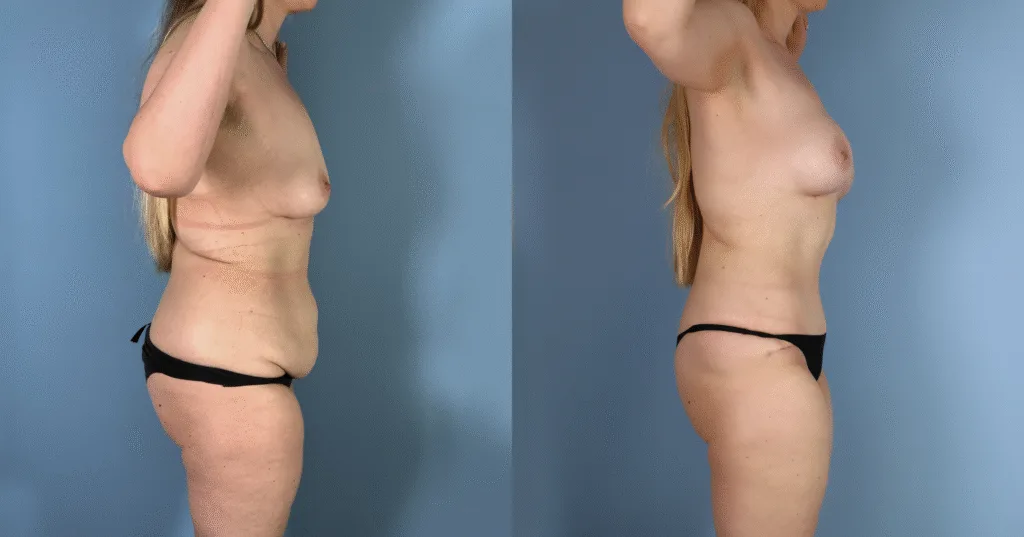
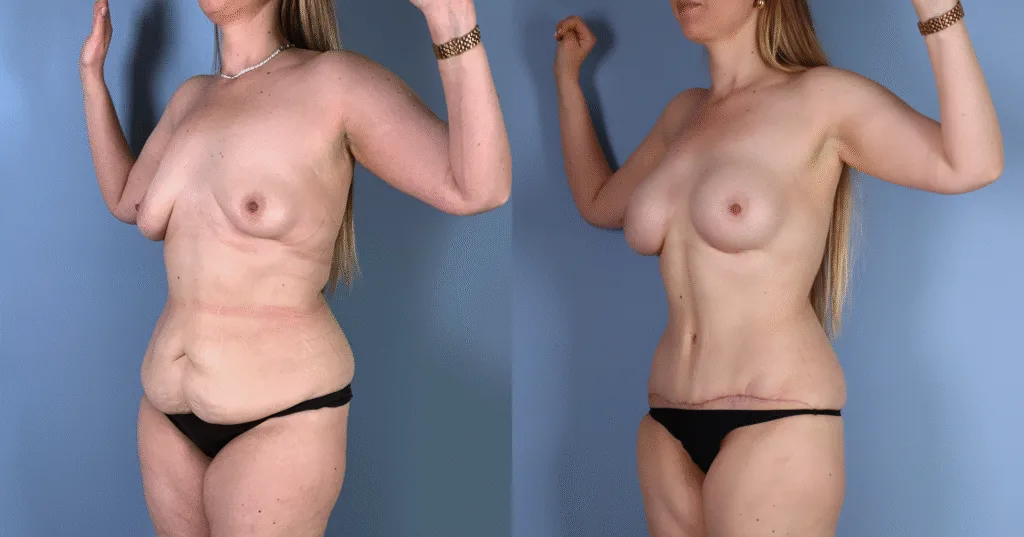
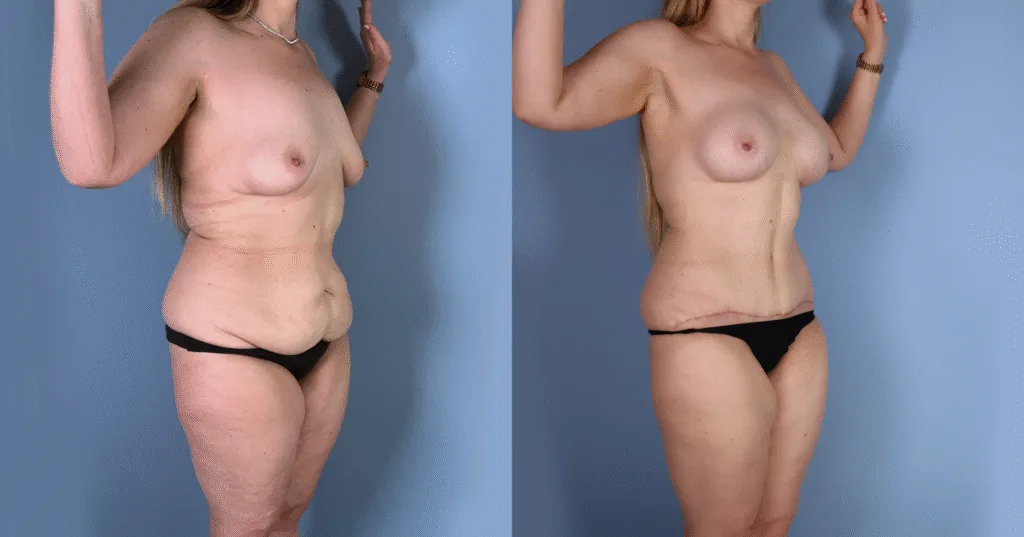
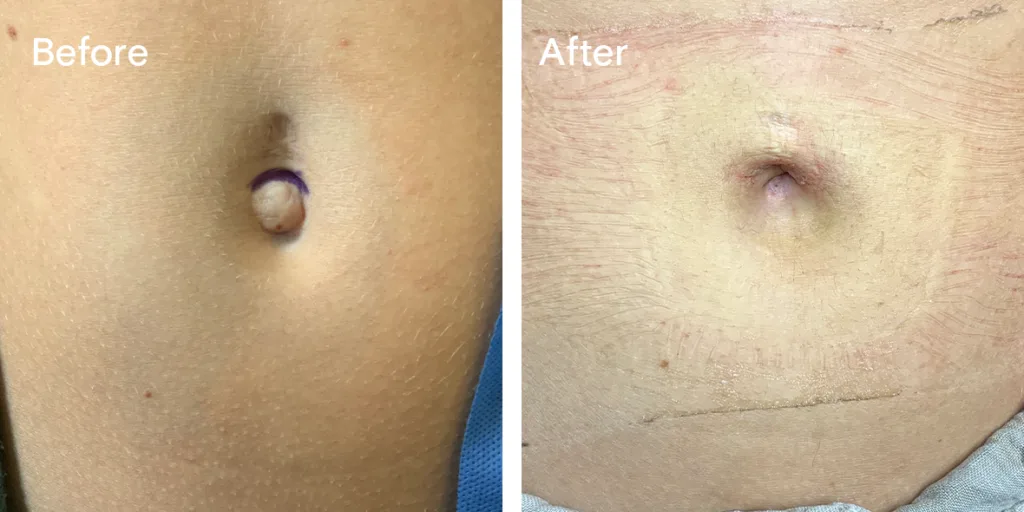
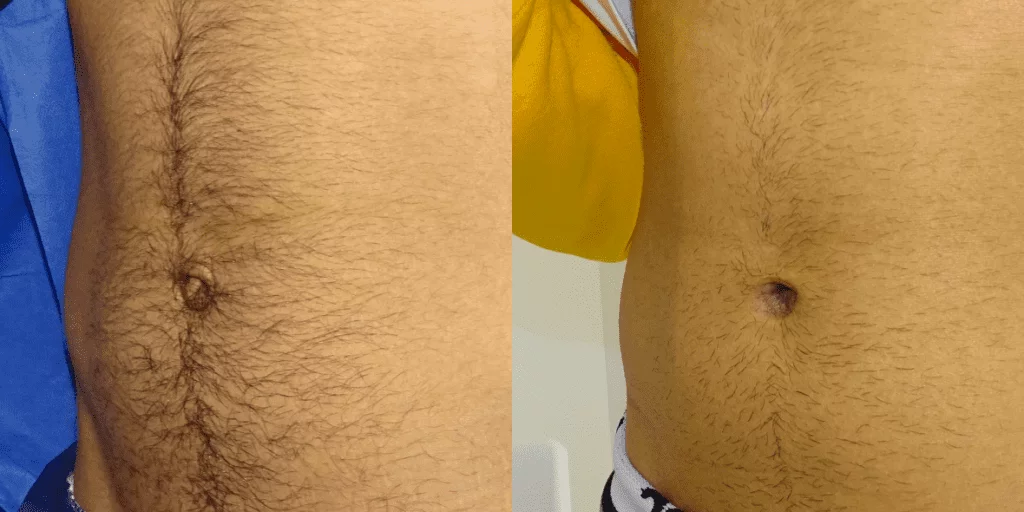
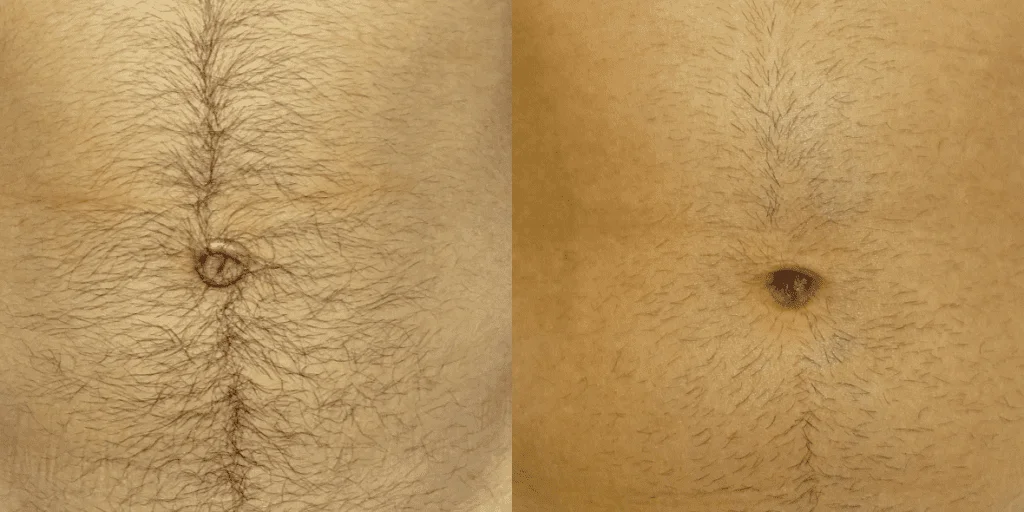
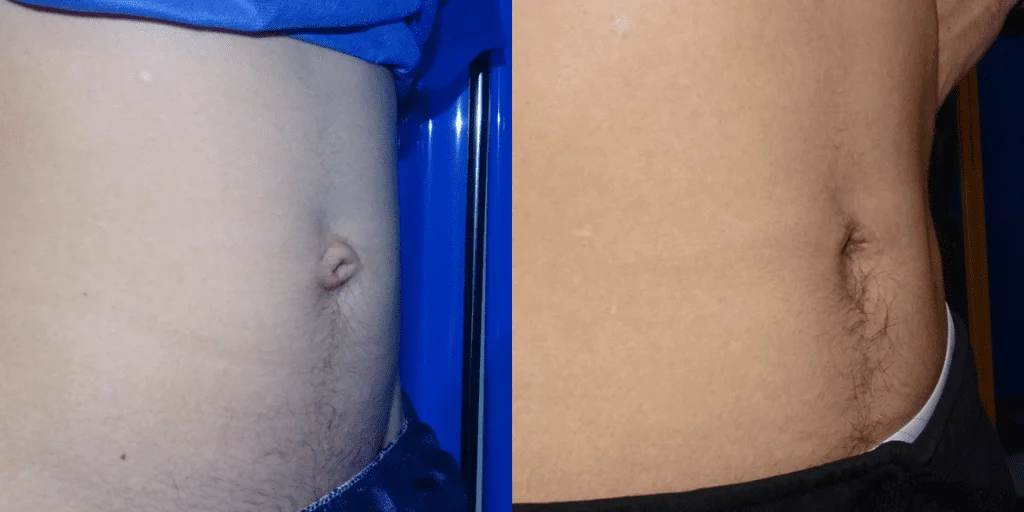
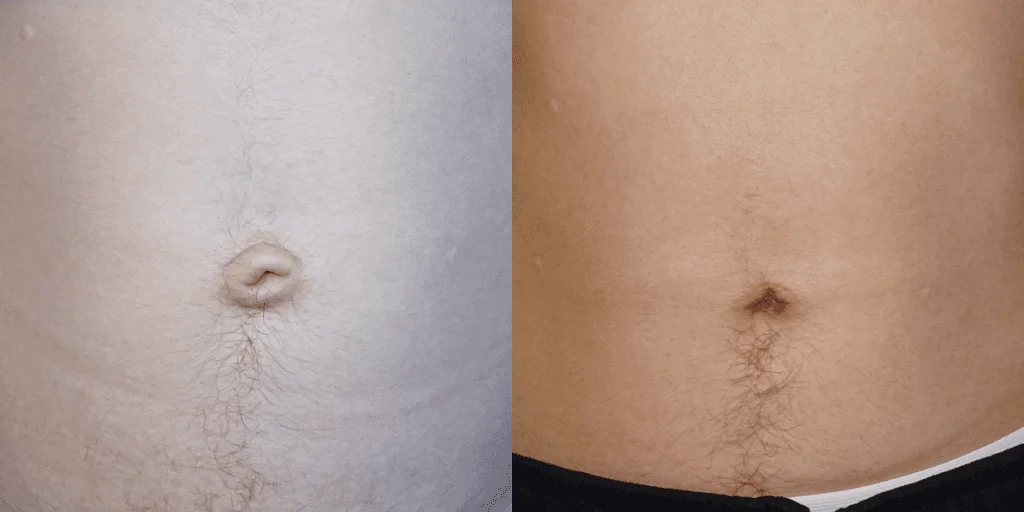
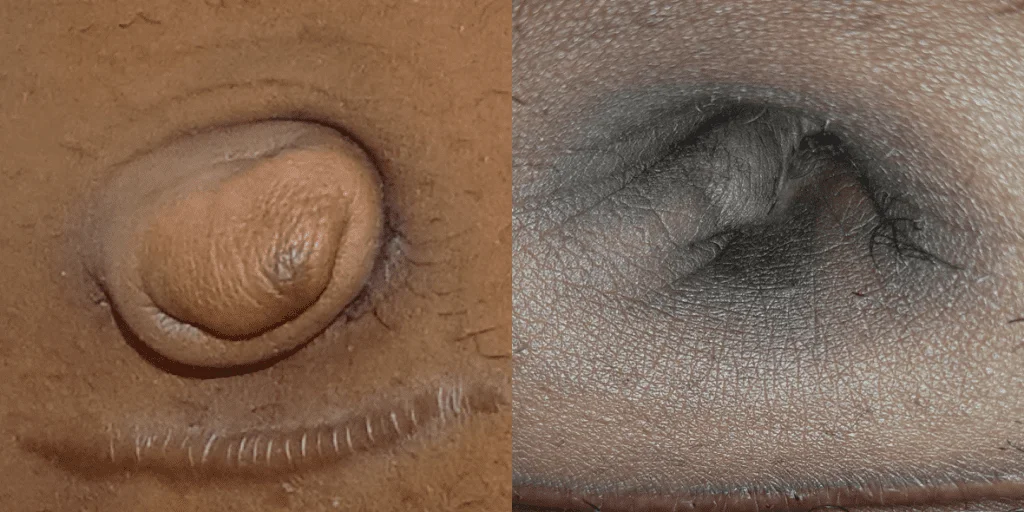
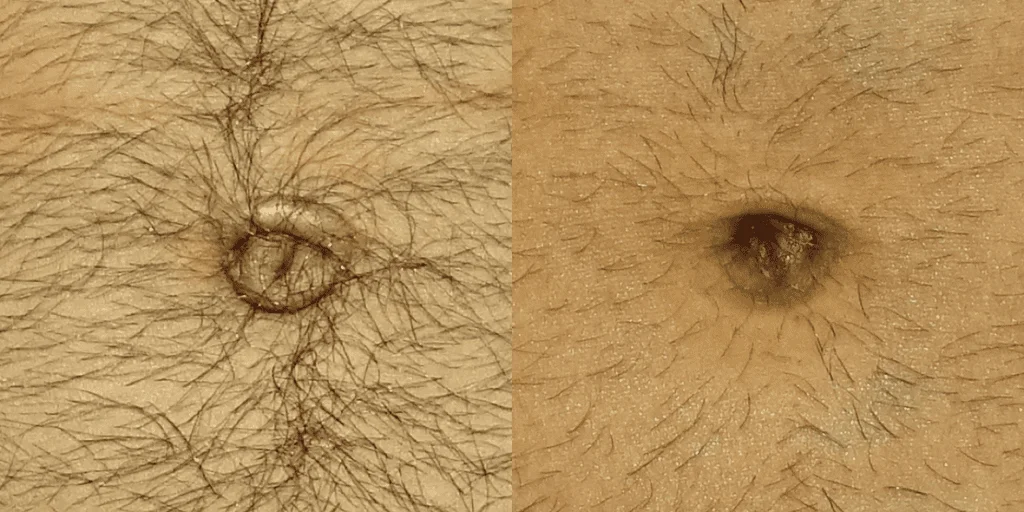
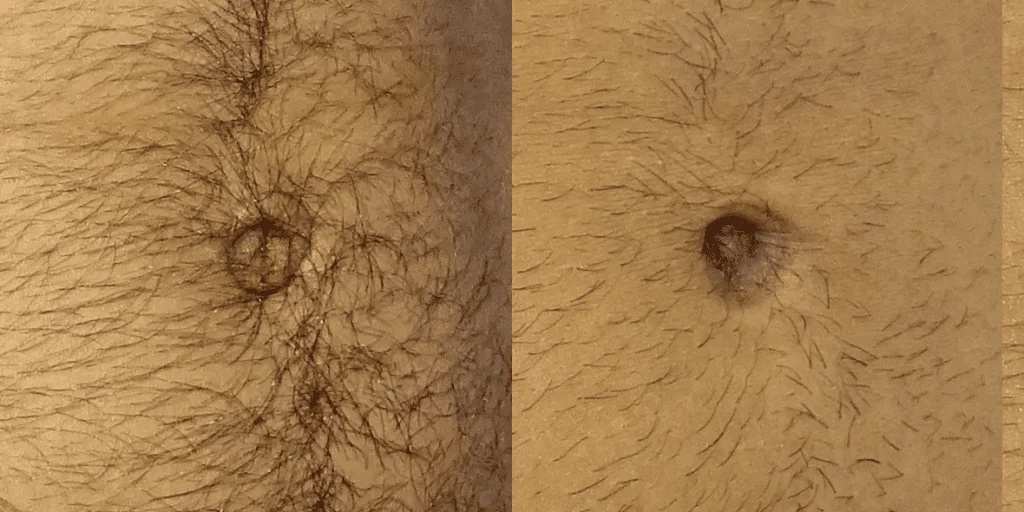
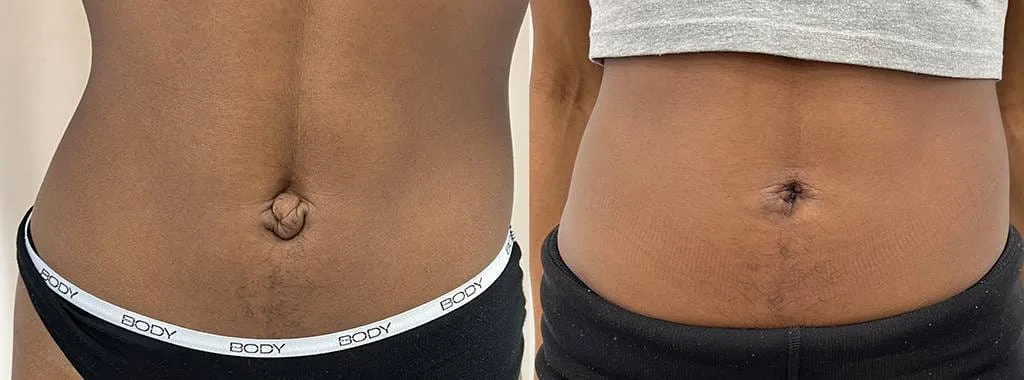
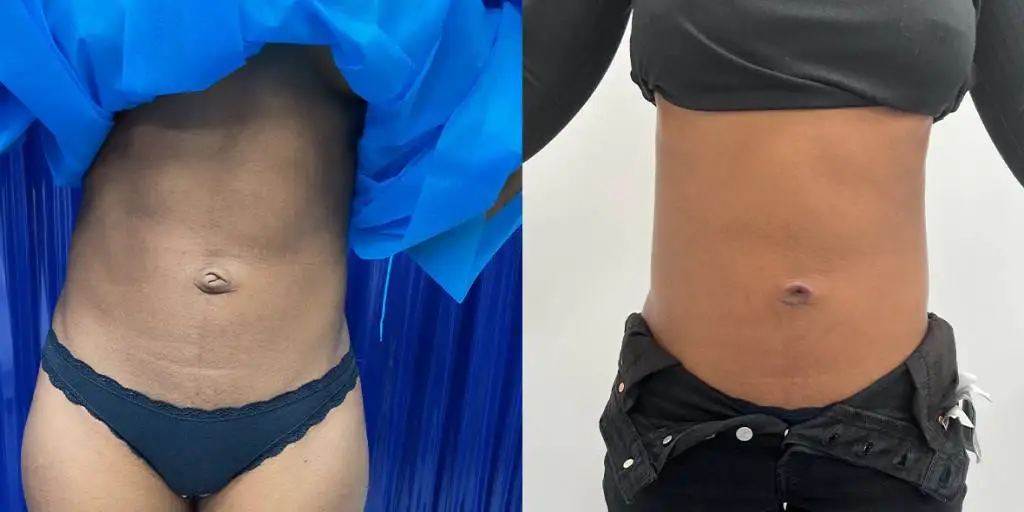
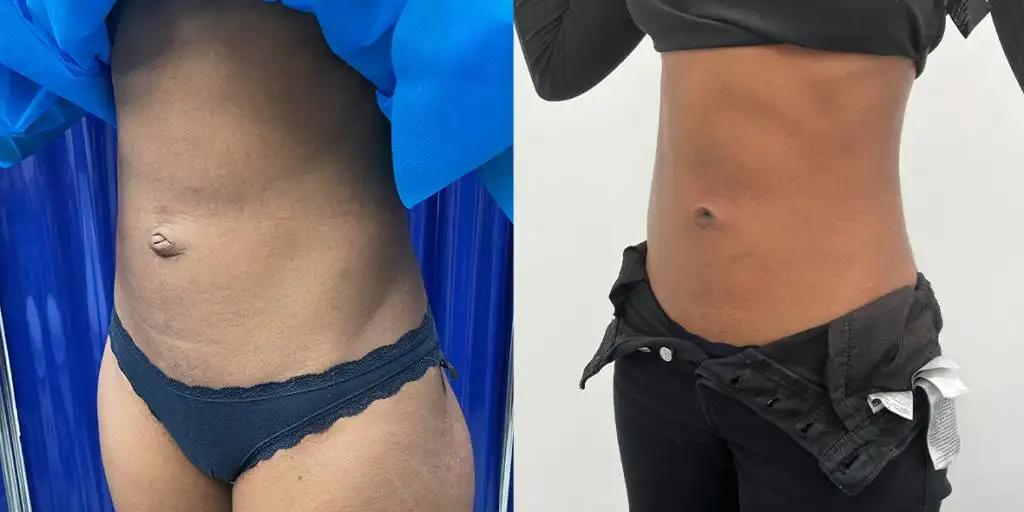
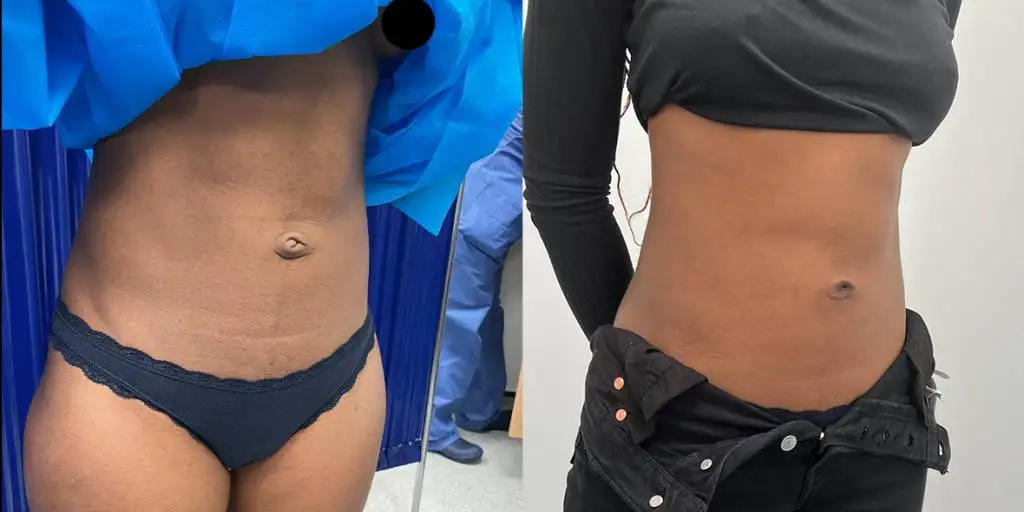
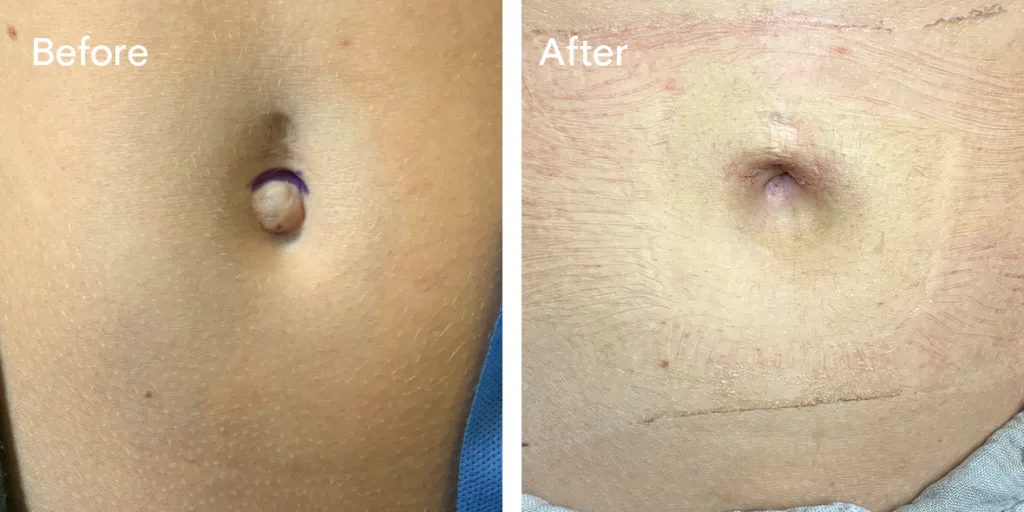
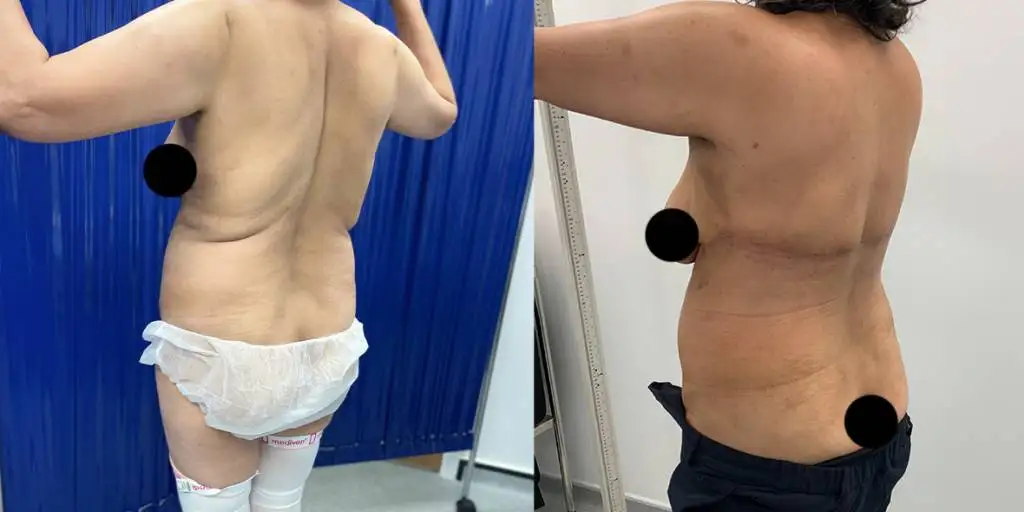
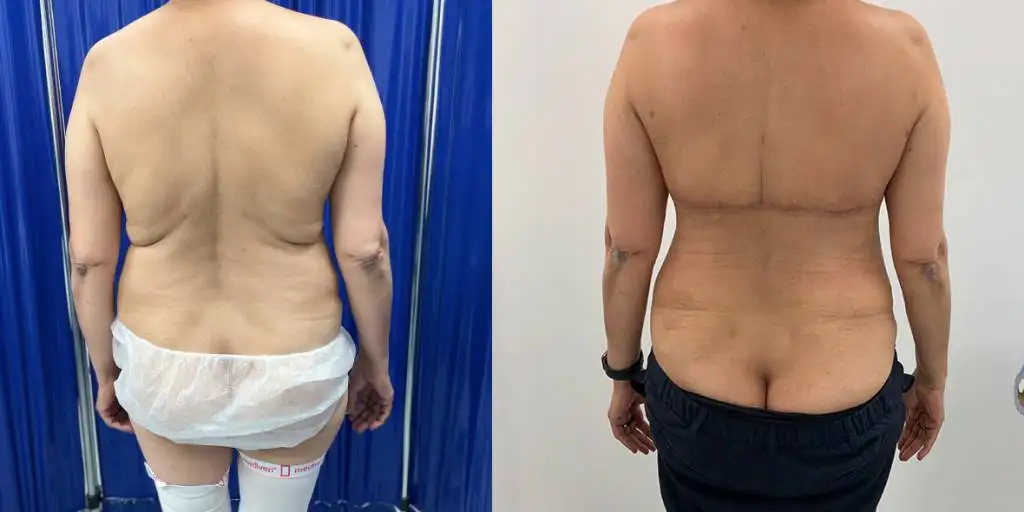
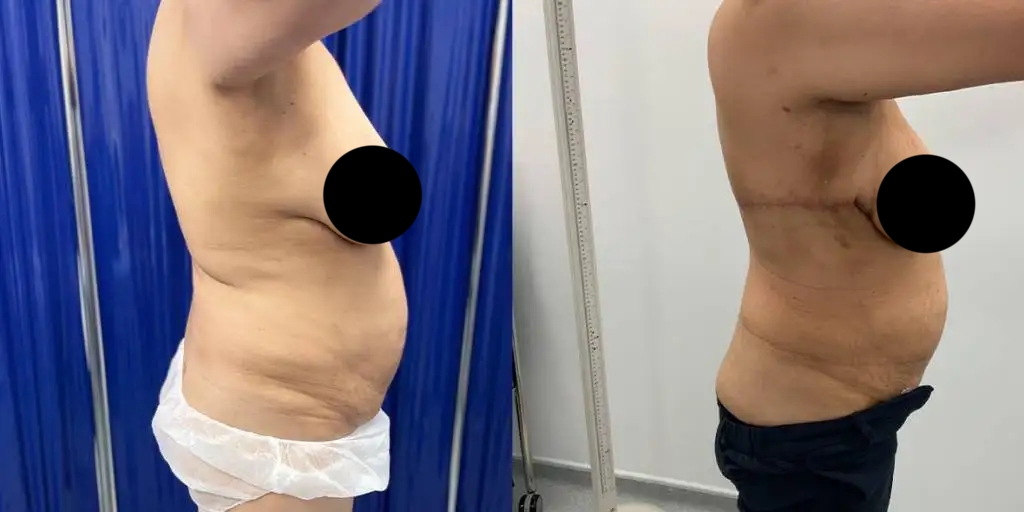
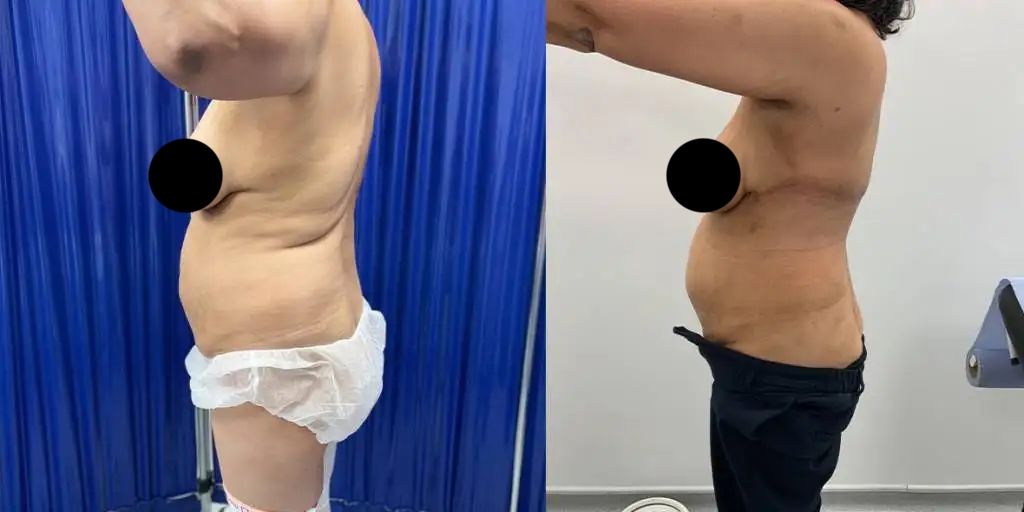
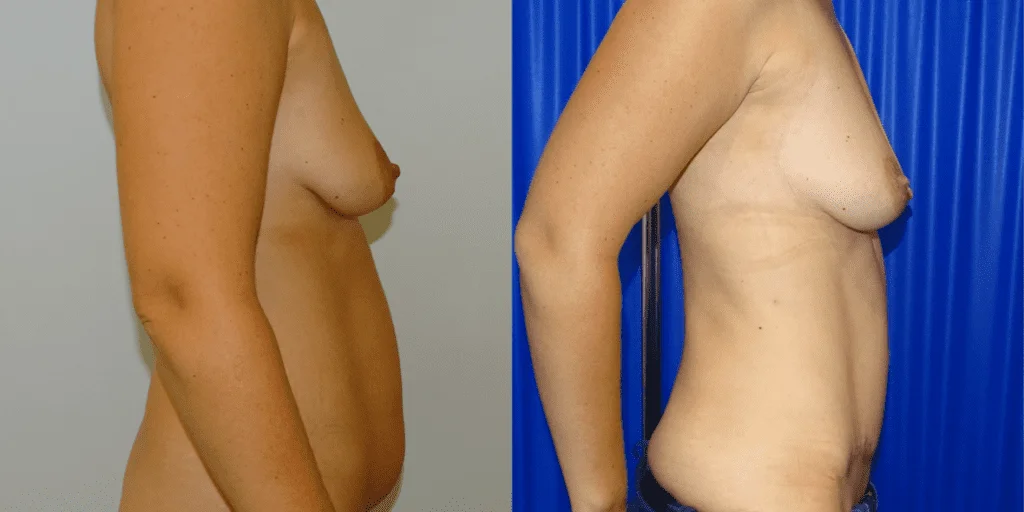
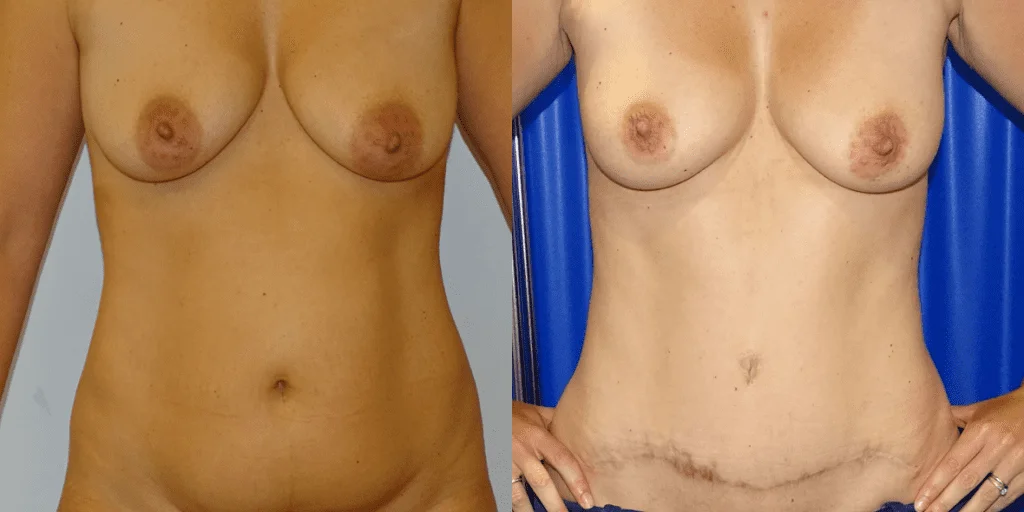
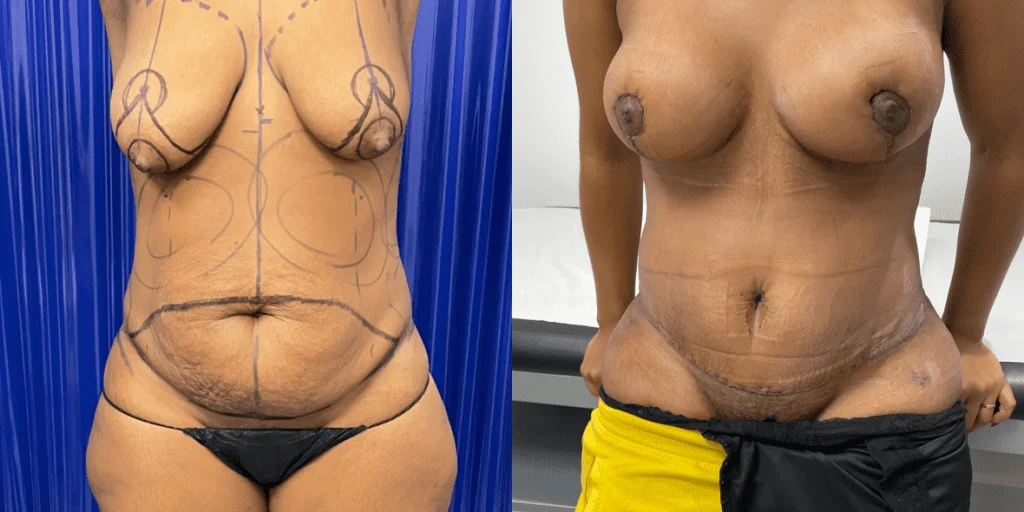
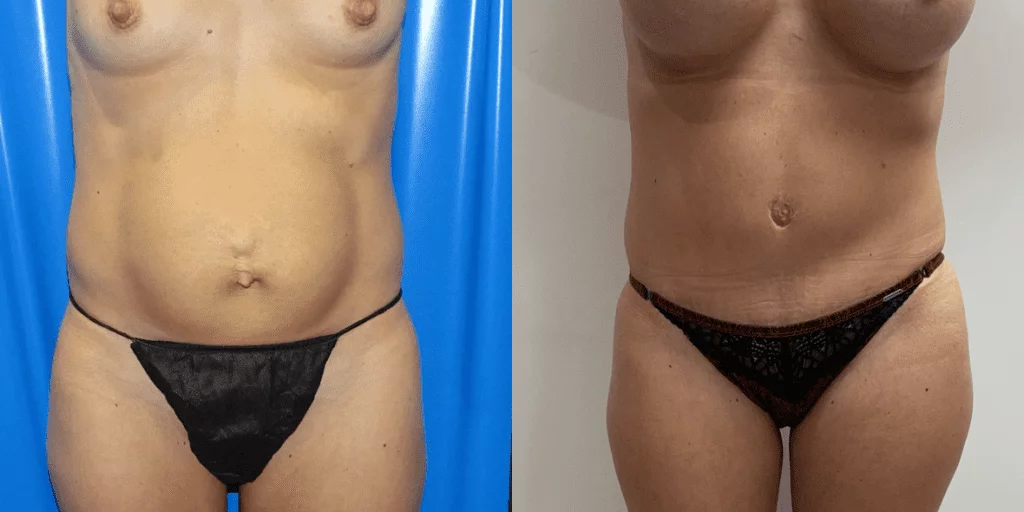
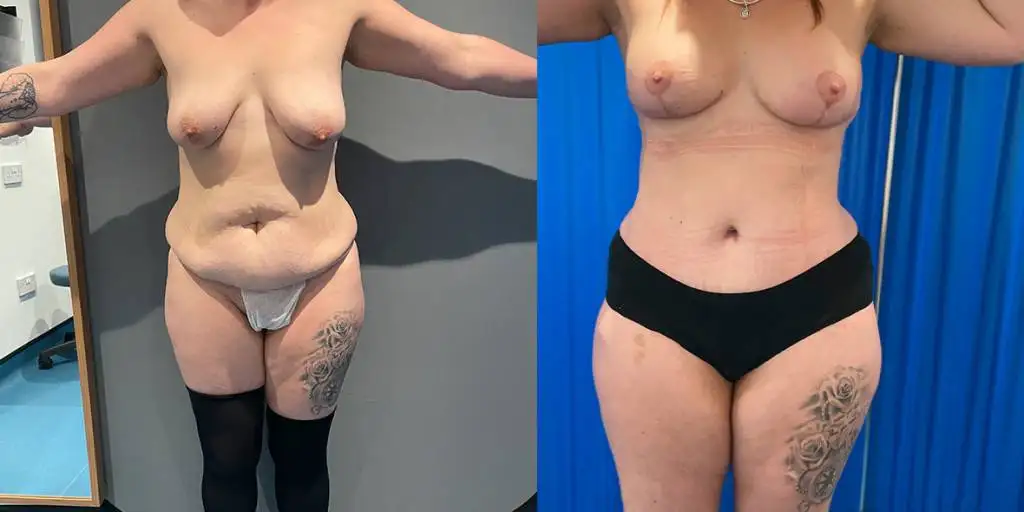
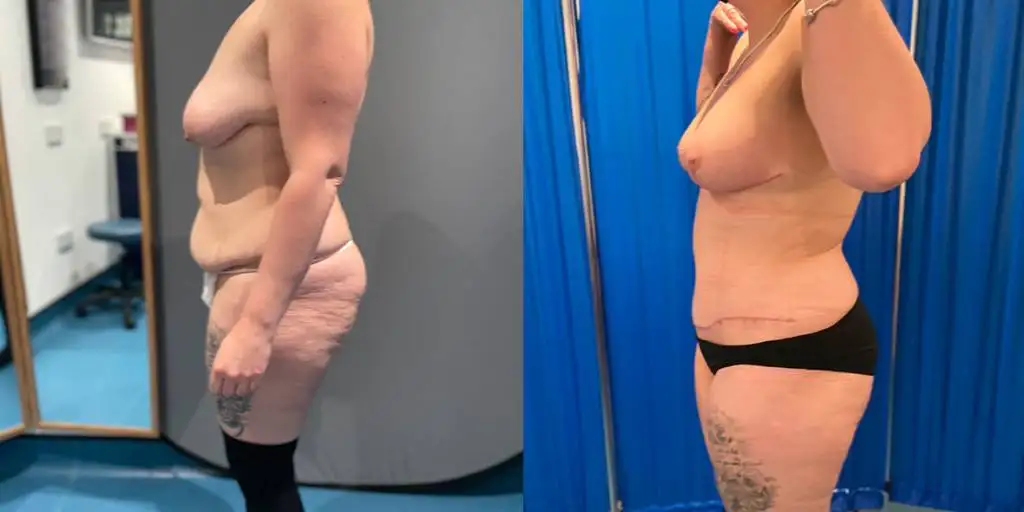
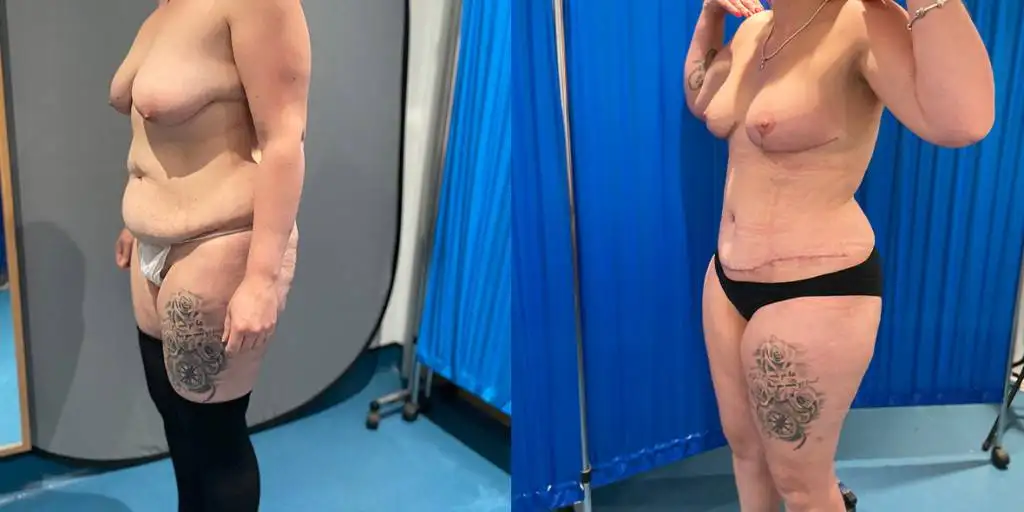
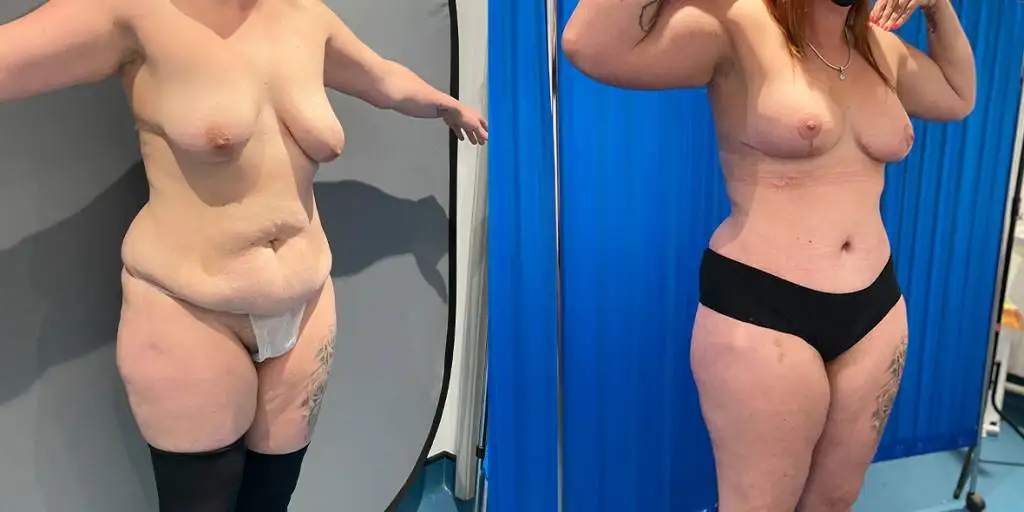
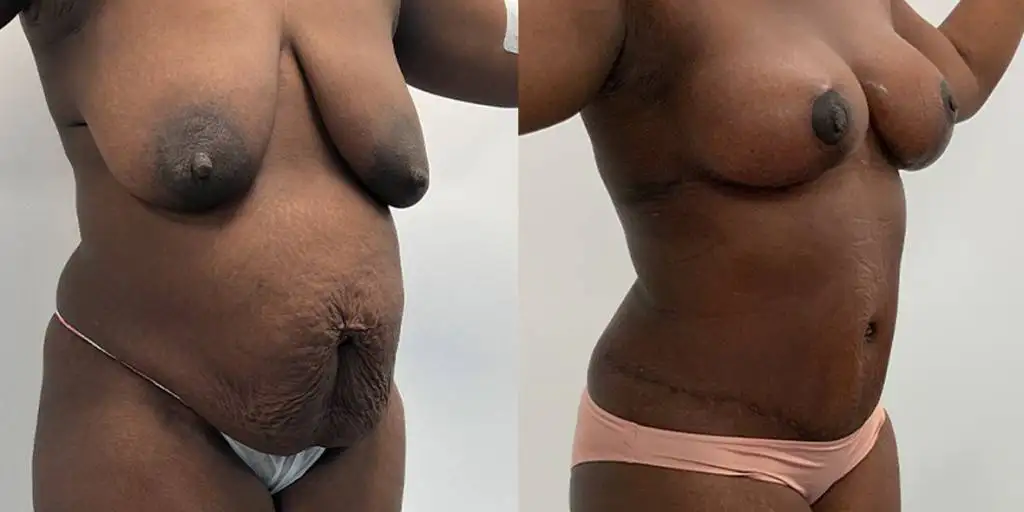
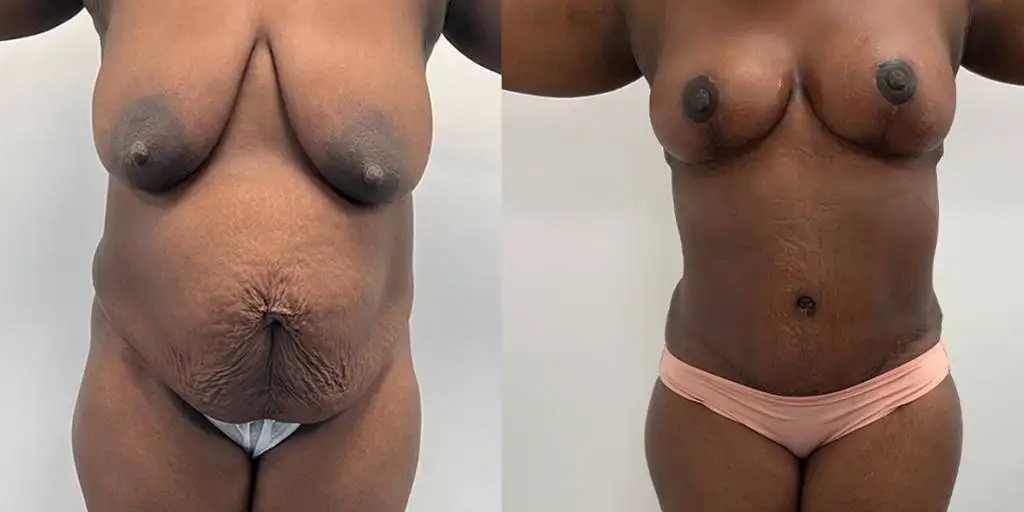
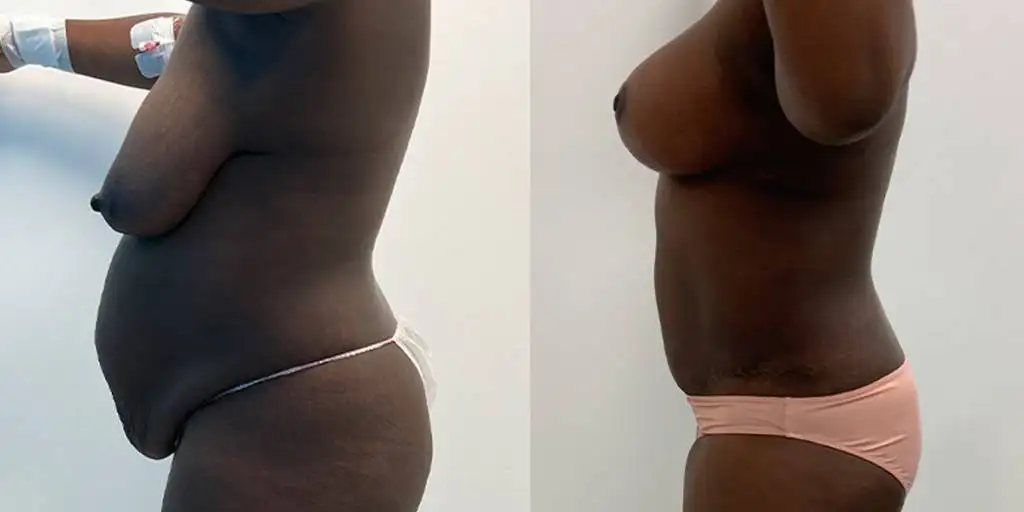
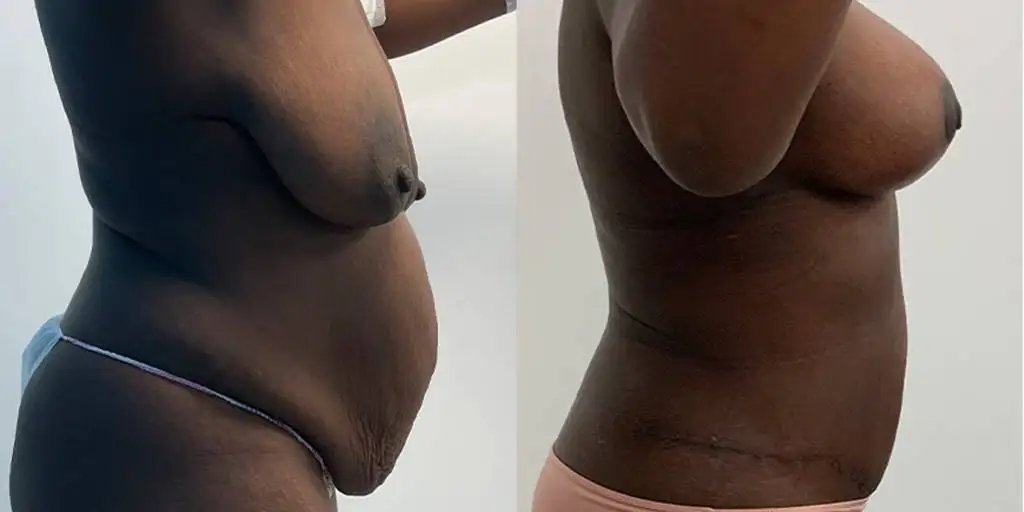
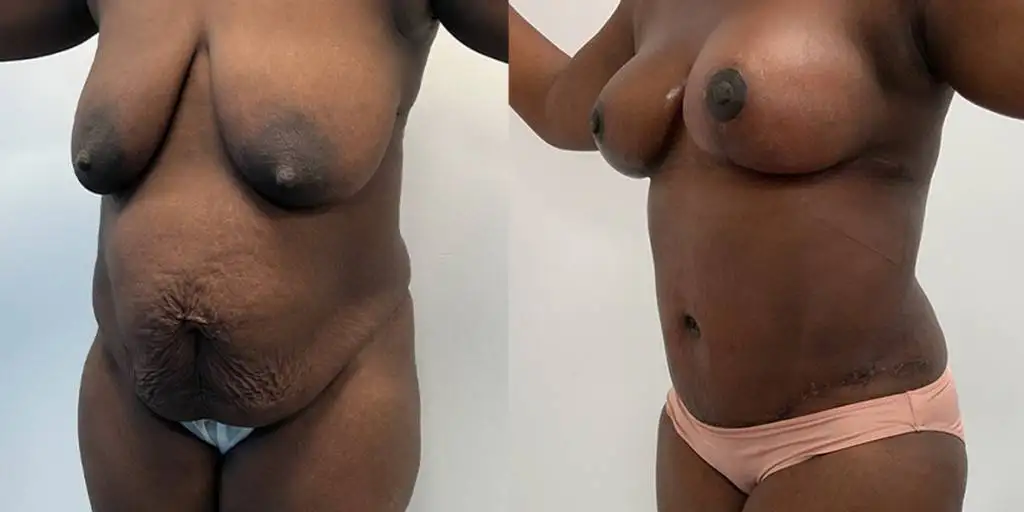
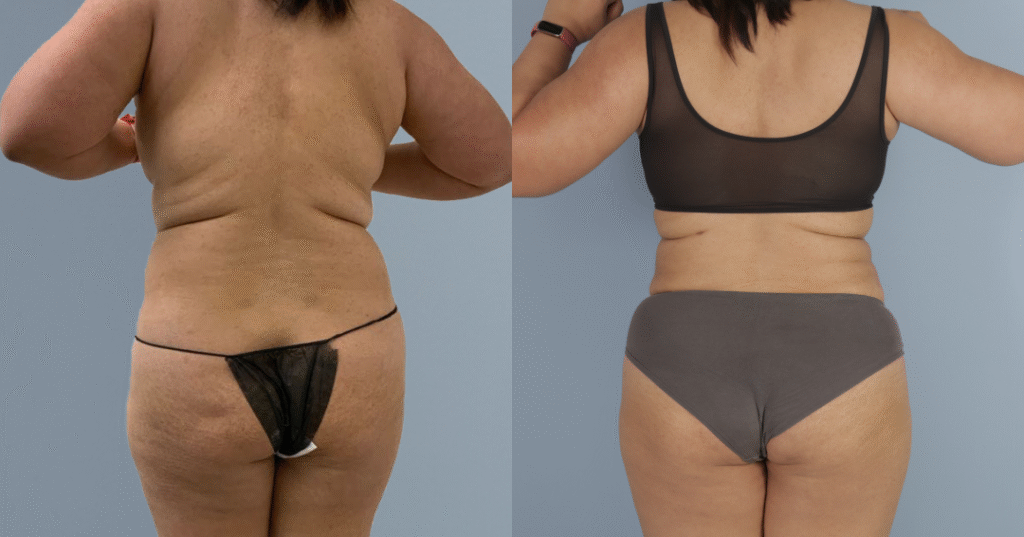
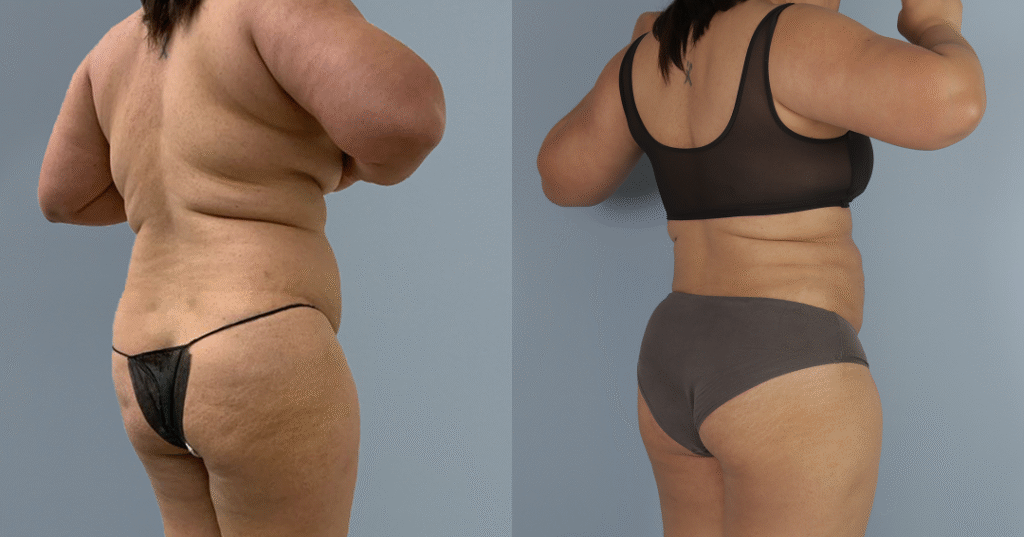
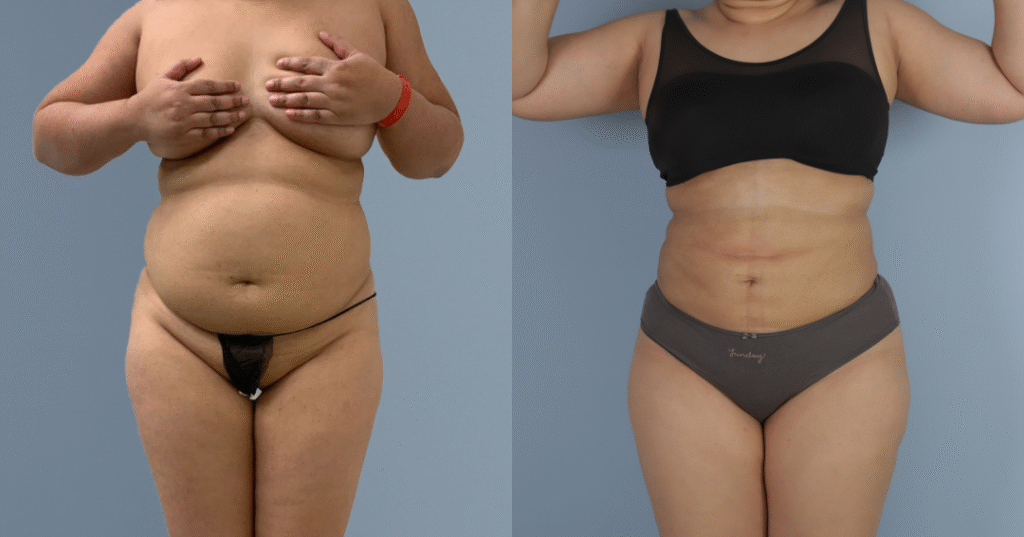
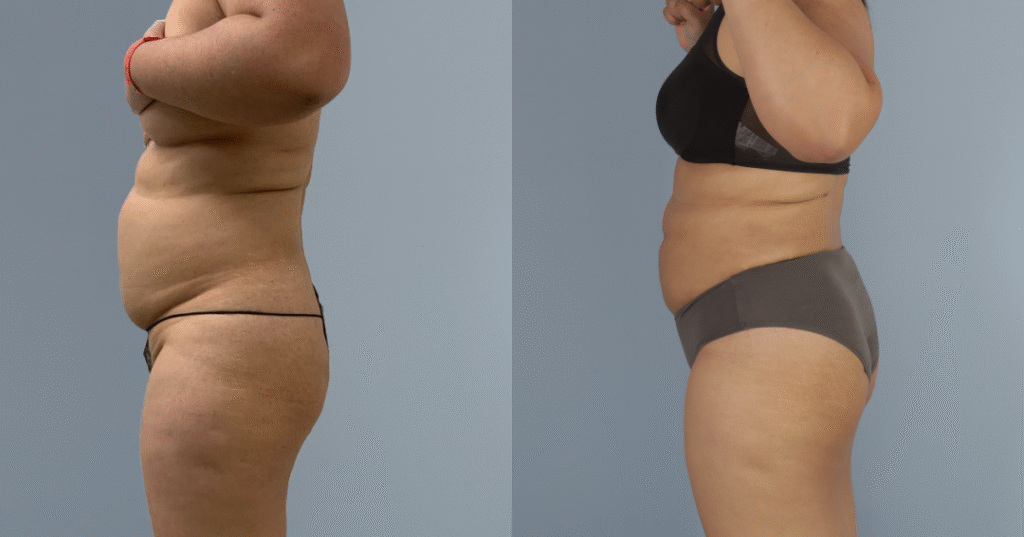
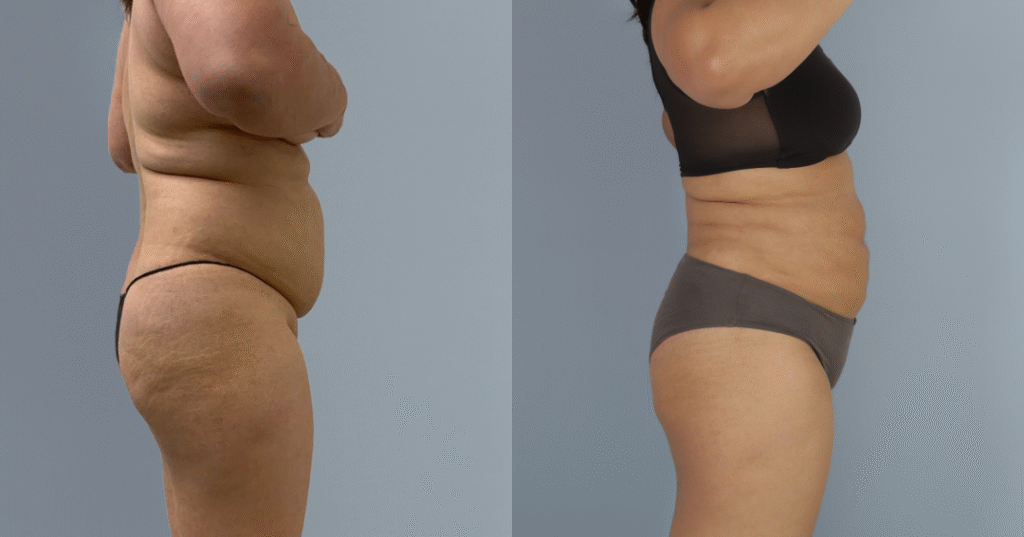
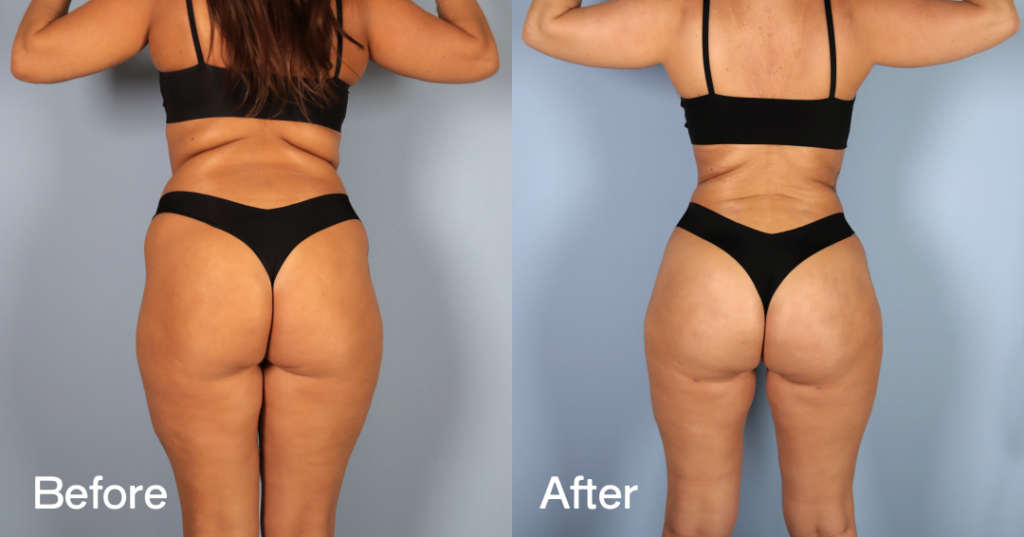
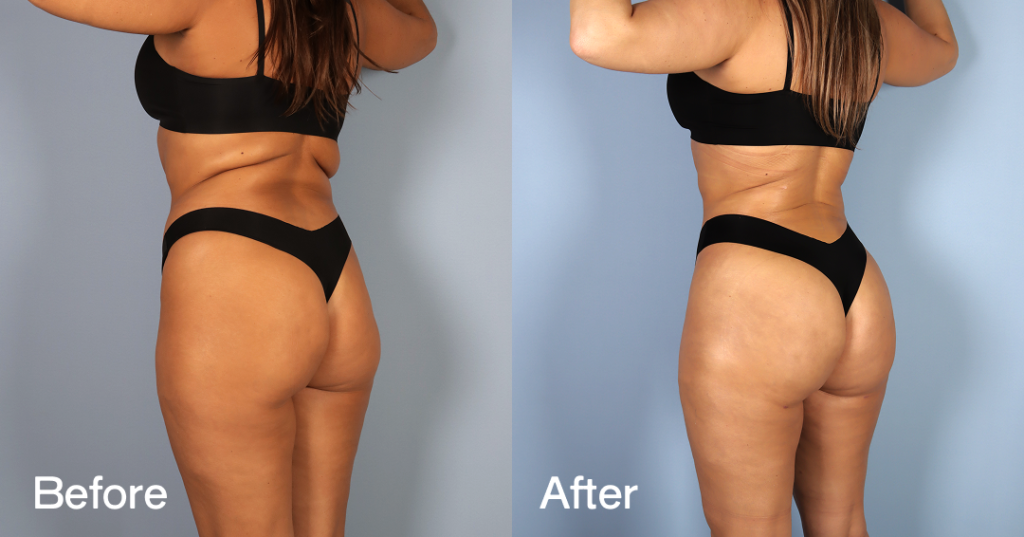
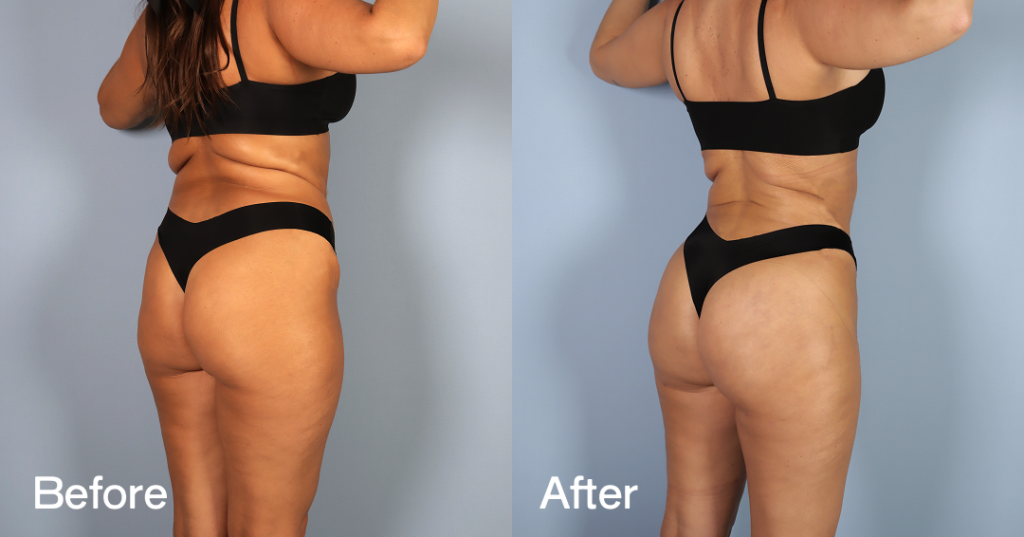
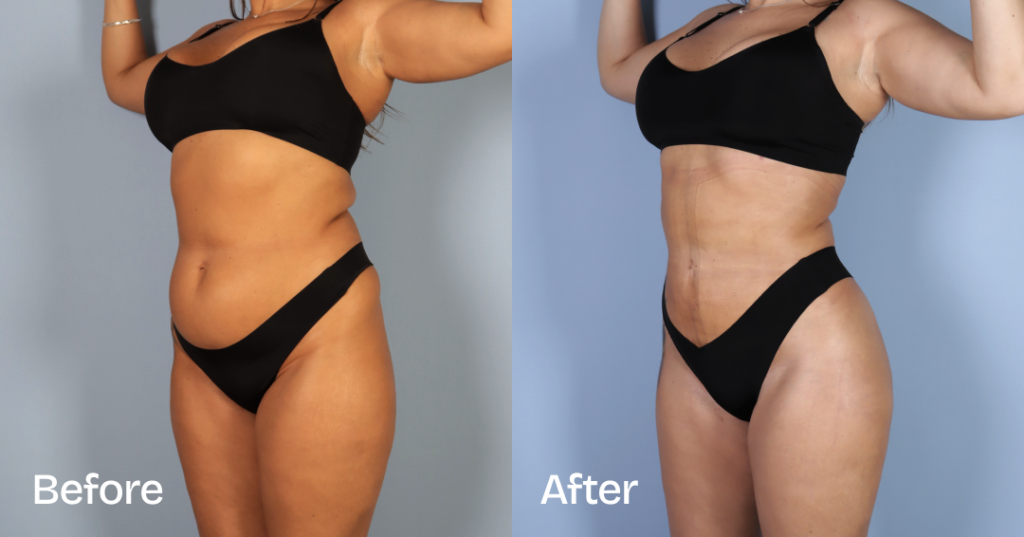
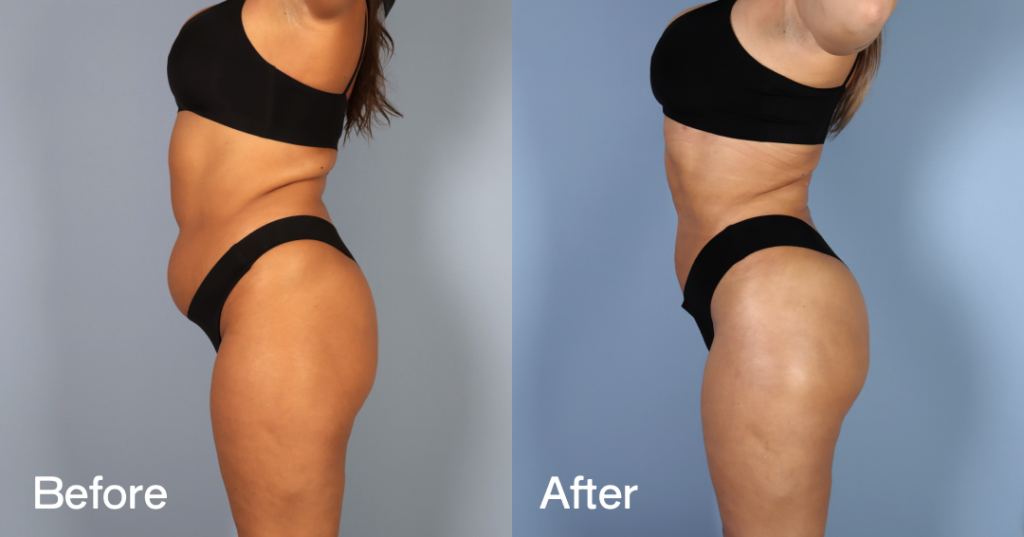
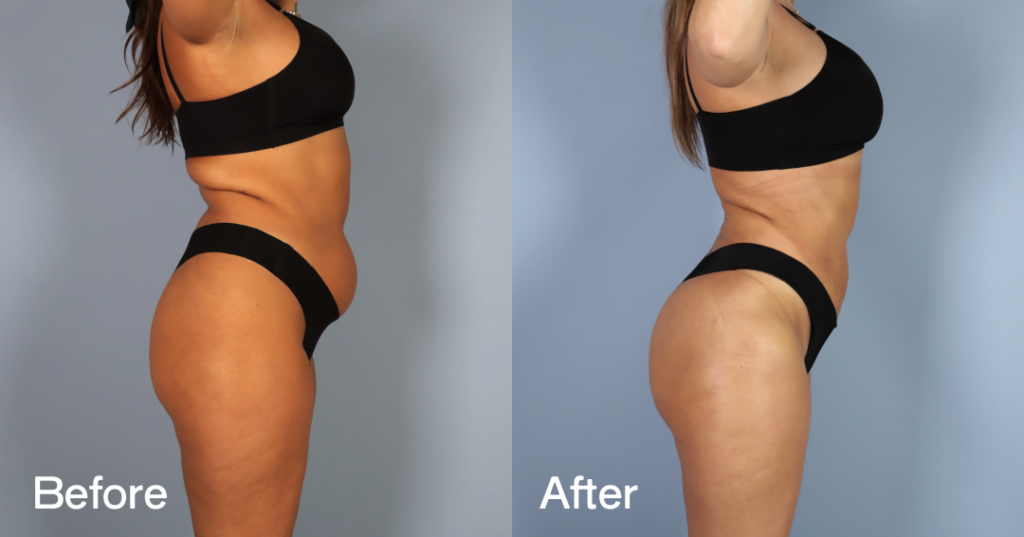
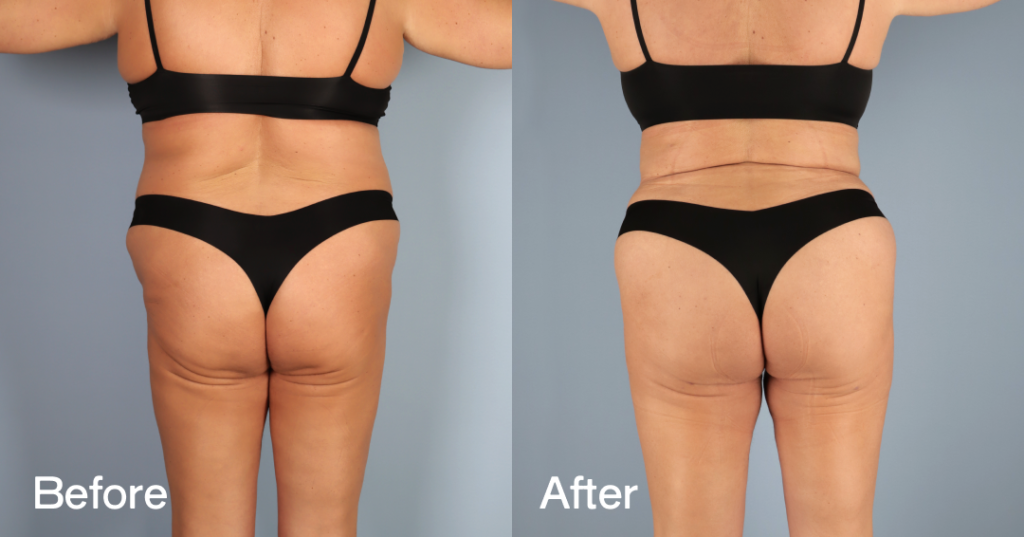
Before and after results
The gallery below shows the real outcomes of CREO Clinic panniculectomy patients. The images show examples of patient outcomes, but results vary from person to person.
Benefits of the panniculectomy
There are potential benefits to a panniculectomy surgery, primarily related to the removal of excess lower abdominal tissue.
The key benefits are:
- Relief from physical discomfort caused by overhanging abdominal skin, such as chafing, limited mobility, and skin infections or irritation
- Removal of stretch marks within the excised skin fold, where present
- A change in abdominal profile through the removal of a protruding skinfold, with outcomes varying based on individual anatomy and surgical scope
The CREO APEX Recovery System
What to expect before, during and after surgery
Clear, careful planning means all CREO surgeries are mapped out in detail. This allows for greater consistency and helps to maintain replicable processes that patients can understand in advance. Your panniculectomy will closely follow the stages below:
Your initial consultation with Dr Tillo is the first step. He will assess suitability, carry out relevant examinations, and define a surgical plan based on your individual presentation.
On the day of the surgery, you are admitted for preparation and review. Following general anaesthesia, the procedure is performed, typically lasting between 2 – 3 hours, although this can vary depending on surgical complexity.
After surgery, you are monitored until it is clinically appropriate for discharge, which may be the same day or require an overnight stay.
Swelling, bruising, and tenderness are expected in the early stages. These symptoms generally improve over time, with many patients returning to routine daily activities within approximately 6-8 weeks. A return to more strenuous activity may take longer, depending on individual recovery.
An initial change in abdominal contour is visible following surgery; however, swelling can persist and gradually settle. Final results typically become clearer over several months, often around six months, although this can vary.
Scarring matures over time, often over a period of up to two years. Ongoing monitoring and appropriate post-operative care may support scar progression, depending on individual healing response.
Risks, limitations and considerations
As with any surgical procedure, panniculectomy carries inherent risks. These risks vary between individuals and are influenced by factors such as general health, body composition, and the extent of surgery. They are discussed in detail during your consultation to support informed decision-making.
Some potential risks are:
- Wound infection
- Delayed or poor wound healing
- Seroma (fluid accumulation)
- Changes in skin sensation or nerve-related symptoms
The limitations of a panniculectomy will also be explained during your clinical assessment. Scarring is an expected outcome due to the nature of the incisions, and the extent and appearance of scars can vary depending on individual healing and surgical approach.
Following surgery, maintaining long-term weight stability is an important factor in preserving outcomes, although this can be influenced by broader lifestyle and physiological factors.
Cost of panniculectomy surgery
The cost of a panniculectomy at the CREO Clinic reflects the complexity of the surgery. Final pricing is determined on a case-by-case basis, depending on factors such as surgical planning, operative complexity, and the extent of treatment required.
Prices for panniculectomy surgeries start from £10,000.
This price includes:
- Your surgical and anaesthetic fees
- CQC-registered surgical facilities
- Follow-up appointments
- Our APEX aftercare package.
The CREO Clinic offers financing via our partner, Chrysalis Finance. Borrowing is interest-free up to 12 months, with longer-term loans available with subsidised interest. All borrowing is subject to approval.
Why choose CREO Clinic
Patients considering panniculectomy at the CREO Clinic are assessed through a clinically led process focused on suitability, safety, and long-term outcomes, rather than a standardised treatment pathway.
Specialist plastic surgeons
All procedures are performed by surgeons working within their defined area of anatomical specialisation, ensuring that treatment planning and execution are based on focused expertise in body contouring surgery.
Surgeon-led clinical planning
All decisions are made by the operating surgeon following a detailed consultation. Surgical planning is based on clinical findings, patient goals, and risk assessment, with no reliance on pre-set treatment models.
Integrated after-care and recovery
Post-operative care is structured and incorporated into the treatment pathway, with follow-up and recovery support tailored to the individual patient’s progress and clinical needs.
Trusted by patients
Dr Omar Tillo, Medical Director, is a Fellow of the Royal College of Surgeons (FRCS) and a member of the British Association of Aesthetic Plastic Surgeons (BAAPS). His practice focuses on maintaining clinical standards, procedural appropriateness, and consistent surgical oversight.